What is the problem and how much of a problem is it?
The year 1928 set the scene for one of the most significant public health milestones in history – the discovery of penicillin. Described as a wonder drug, the medical world rejoiced at what was hoped would be the decisive blow in the eternal battle between humans and infection. However, not long afterwards, it appeared that the bugs had fought back. In 1940, the first signs of antibiotic resistance became apparent, and by 1942, the spread of resistance was well documented.1
Image. Bacteria grown in a laboratory2
“The rise of antimicrobial resistance is a global crisis, recognised as one of the greatest threats to health today… [it] is a slow-motion tsunami.”
– Dr Margaret Chan, then-Director General of the World Health Organization, 2016.3
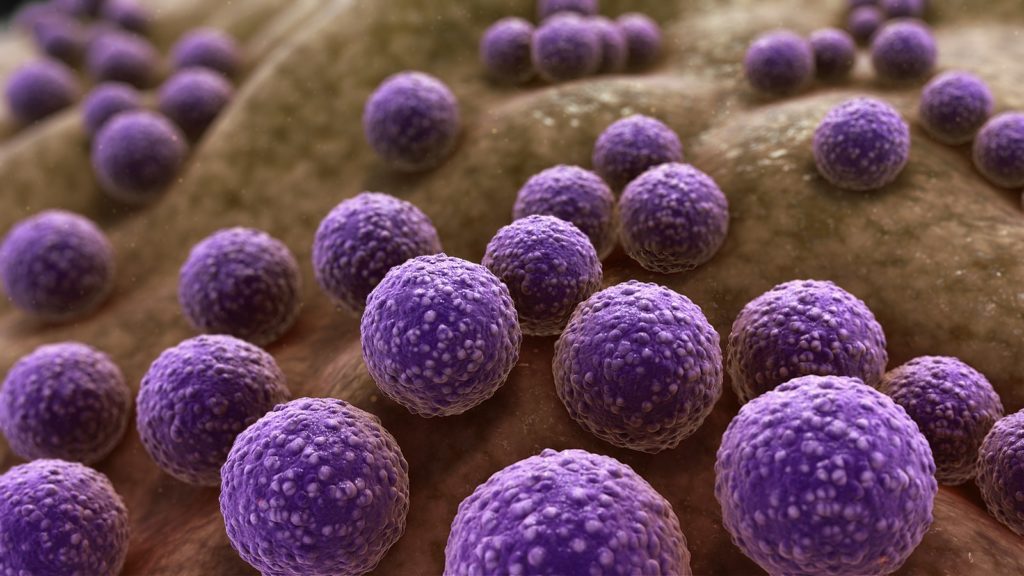
Antimicrobial resistance (AMR) occurs when microorganisms – bacteria, fungi, viruses and parasites – change after being exposed to antimicrobial drugs (such as antibiotics, antifungals, antivirals, antimalarials and anthelmintics). Often, these microorganisms are referred to as ‘superbugs’.4
Alarmingly, it is estimated that around 2.4 million people could die from AMR in Europe, North America and Australia alone, between 2015-2050, if the status quo is maintained.5 AMR threatens all effective prevention and treatments of an ever-growing range of infections, and without effective antibiotics, major surgery and chemotherapy would become too risky. AMR is also an existential threat to efforts aimed at fighting three of the biggest infectious killers in the world – HIV/AIDS, tuberculosis and malaria.4
How did it come to this?
AMR occurs naturally over time, generally through genetic mutations. However, there are certain key drivers that have accelerated, and are continuing to accelerate, the process.4 These include:
- The overuse and misuse of antibiotics
The overuse and misuse of antibiotics are the leading cause of antibiotic resistance, which is the main form of AMR. When we take antibiotics, some bacteria die, but there may be some resistant bacteria that survive and multiply. The more we take antibiotics, the greater the chance bacteria have to develop resistance. In some parts of the world, the use of antibiotics is exceedingly high, resulting in high rates of resistance that can then be easily spread to other regions.6,7
A key driver of the overuse and misuse of antibiotics in Australia is the fact that they are overprescribed. In 2017 for instance, more than 26 million prescriptions for antimicrobials were issued, and in many cases, these were prescribed for conditions in which there is no evidence of benefit (e.g. using antibiotics for the flu).8
- Poor sanitation and hygiene in healthcare settings
Poor sanitation and hygiene practices in healthcare settings can increase the spread of drug-resistant microorganisms, which can lead to prolonged illness and length of hospitalisation for infected patients. Such practices ultimately increase the need for antibiotics, as patients might need to be treated for infections that are entirely preventable.7 Alarmingly, 1 in 10 adult patients with acute illness, develop a healthcare-associated infection when in hospital, with a high number of these resulting from drug-resistant microorganisms.9
Get on top of your general health
Find and instantly book affordable GPs within Australia
What exactly is the ‘golden staph’ superbug?
- Antimicrobial usage in food production
Uncontrolled use of antibiotics for the control and treatment of disease in livestock, as well as for growth stimulation purposes, is a significant driver of AMR. This can affect humans through the consumption of poorly cooked foods, as well as through the consumption of food crops contaminated by livestock faeces. Resistance can also be spread directly to those in contact with the animals.10
Worldwide, the majority of antimicrobials are not consumed by humans, but by animals for purposes of food consumption. Antibiotics are only used to treat animals in a small number of cases. Instead, much of its use is either prophylactic (when used in healthy animals to prevent infection) or for growth promotion.11,12
How do antibiotics promote animal growth?
The use of enormous quantities of antimicrobials in food production, and its widespread release into the environment through animal sewage and runoff from agricultural sites, is a significant contributing factor to the development and spread of resistant zoonotic bacteria. These are bacteria which spread between animals and humans, and they are linked to food-related human disease (e.g. foodborne gastroenteritis from Salmonella bacteria).12
Find out more about foodborne disease outbreaks in Australia
- Other non-human uses of antimicrobials
Antimicrobials and their additives are also widely used in domestic pets, plant agriculture (e.g. fruit, vegetables and orchids) and industrial applications such as oil pipelines and industrial paints.12
What can we do about it?
The Australian Government Department of Health and Department of Agriculture and Water Resources have six key tips on how we can help to reduce antibiotic resistance:13
- Wash your hands regularly to help prevent infections and keep up to date with vaccinations.
- Wash fruits and vegetables and cook food properly to prevent food-related infections.
- Educate yourself on what antibiotics can, but just as importantly, can’t do. For instance, antibiotics only work against bacteria, and do not work against colds and flus (which are caused by viruses).
- Don’t pressure your health professional for antibiotics if they say that they are not needed. Ask about other things that may help alleviate your symptoms.
- Don’t use antibiotics that were not prescribed for you, and don’t use leftover antibiotics. Only take antibiotics when they are prescribed for you.
- Always follow your health professional’s instructions when taking your prescribed antibiotics.
References
- Lobanovska, M; Pilla, G. 2017. Penicillin’s Discovery and Antibiotic Resistance: Lessons for the Future? Yale J Biol Med 90(1): 135-145. Full article available from: URL link
- Wikipedia (online). Small intestinal bacterial overgrowth and related image [accessed 12 Sep 2019]. Available from: URL link
- WHO (online). WHO Director-General briefs UN on antimicrobial resistance 2016 [accessed 11 Sep 2019]. Available from: URL link
- WHO (online). Antimicrobial resistance [accessed 11 Sep 2019]. Available from: URL link
- OECD (online). Stemming the Superbug Tide [accessed 11 Sep 2019]. Available from: URL link
- WHO (online). Report on Surveillance of Antibiotic Consumption [accessed 11 Sep 2019]. Available from: URL link
- Australian Government (online). Antimicrobial resistance [accessed 11 Sep 2019]. Available from: URL link
- ABC News (online). Antibiotic resistance still poses substantial risk despite fall in antibiotic use, report finds [accessed 11 Sep 2019]. Available from: URL link
- The Conversation (online). 1 in 10 patients are infected in hospital, and it’s not always with what you think [accessed 11 September 2019]. Available from: URL link
- FAO (online). Antimicrobial Resistance [accessed 11 September 2019]. Available from: URL link
- The Review on Antimicrobial Resistance (online). Antimicrobials in Agriculture and the Environment: Reducing Unnecessary Use and Waste [accessed 11 September 2019]. Available from: URL link
- WHO (online). Antimicrobial resistance: Antimicrobial use [accessed 11 Sep 2019]. Available from: URL link
- Australian Government (online). Antimicrobial resistance: What you can do [accessed 11 Sep 2019]. Available from: URL link
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.