- What is Placenta Accreta?
- Statistics
- Risk Factors
- Progression
- Symptoms
- Clinical Examination
- How is it Diagnosed
- Prognosis
- Treatment
- References
What is Placenta Accreta?
Placenta accreta is a potentially life threatening obstetric condition in which the placenta is abnormally attached to the uterus. This can lead to massive blood loss during or following delivery. This is thought to result from a defect in the layer of tissue that would normally separate the placenta from the uterus (deciduas basalis). As a result, projections of the placenta (chorionic villi) are able to invade the uterus to varying degrees.
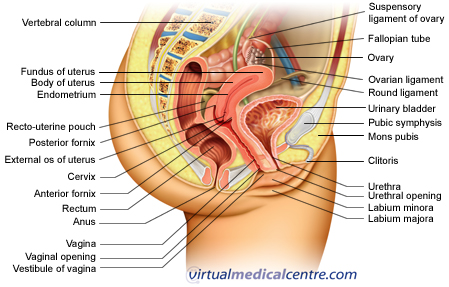
While placenta accreta is often used as a general term to describe this condition, more specifically it refers to the presence of chorionic villi on the inner (myometrial) surface of the uterus. Where the chorionic villi invade the deeper muscular layer (the myometrium), this is termed placenta increta. Where infiltration occurs through the myometrium with or without infiltration of adjacent structures including the bladder this is termed placenta percreta.
Statistics
Although the condition was quite rare 30 years ago, the incidence of placenta accreta has been steadily increasing, mirroring increased rates of caesarean section delivery, which is one of the principle risk factors for placenta accreta.
Currently, placenta accreta occurs in approximately 1 in 2,500 deliveries.
Risk Factors
Placenta accreta most commonly occurs in the setting of placenta praevia with previous uterine surgery including caesarean section. In women with a previous caesarean section and current placenta praevia, the risk of placenta accreta is 25%. For women with two or more previous caesarean sections, this risk rises to 40%.
Other predisposing factors have been identified including:
- Advanced maternal age
- Increased parity (number of pregnancies beyond 20 weeks gestation)
- Unexplained elevated maternal serum alpha-fetoprotein
- Smoking
- Uterine myomas
- Asherman’s syndrome
Progression
During the pregnancy, the placental tissue can invade the different layers of the uterus to varying degrees. The main concern is that following delivery of the baby the placenta will fail to separate from the uterus with the potential for massive, life threatening blood loss.
Symptoms

More information on postpartum haemorrhage
Clinical Examination
There is very little for a doctor to find on clinical examination of a woman with placenta accreta.
Instead the doctor will be interested in your previous obstetric history including details about previous caesarean sections/uterine surgery and the location of the placenta in the current pregnancy if known. This information is especially important given that placenta accreta most frequently occurs in women with a current placenta praevia and a history of uterine surgery.
How is it Diagnosed
Where a diagnosis of placenta accreta is suspected, investigations including ultrasound and magnetic resonance imaging (MRI) are required to determine risk.
Ultrasound
Magnetic resonance imaging
MRI can be used to diagnose placenta accreta. However, in certain cases where the placenta accreta is located posteriorly (towards the back), it is often no better than ultrasound. Furthermore, MRI is costly and not readily accessible.
Maternal serum alpha fetoprotein
Placenta accreta should also be suspected in pregnant women with elevated maternal serum alpha-fetoprotein (MSAFP) levels, with no other obvious cause. This is a protein found in the blood, at highest concentrations in the foetus. The defect in the layer normally separating the placenta and uterus allows leakage of foetal alpha-fetoprotein into the mother’s circulation. Up to 45% of women with placenta accreta have elevated MSAFP levels in the absence of an obvious cause.
Prognosis

Some of the complications that accompany hysterectomy include the need for blood transfusion, infection, injury to nearby tissues/organs and the formation of fistulas. As hysterectomy involves the surgical removal of the uterus, it means that the woman would no longer be able to bear children.
The rate of complications is minimised by performing the surgery as an elective procedure rather than in an emergency situation. Where the diagnosis is made during the pregnancy, planning the delivery at a suitable hospital with appropriate facilities such as obstetric anaesthesia, appropriate surgical expertise and an intensive care unit also helps to minimise adverse outcomes.
Treatment
Maternal counselling should include discussion pertaining to the choice and timing of an elective delivery, whether to make an attempt to separate the placenta at the time of delivery, the use of radiological interventions in an attempt to minimise blood loss and the use of particular drugs post-delivery.
Delivery of a woman with a diagnosis or suspicion of placenta accreta should take place in a hospital with adequate facilities for high volume blood transfusion, interventional radiology and specialist obstetric, anaesthetic and intensive care. Prior consultation with urology (specialist of the urinary system) and gynaecology oncology specialists (specialists of gynaecological cancer) may be appropriate and these specialists should be close at hand. Women with placenta accreta should reside close to the designated hospital throughout the third trimester of pregnancy in case of spontaneous labour, antepartum haemorrhage or other complications.
Effectively there are three treatment options including:
- Total abdominal hysterectomy – generally accepted as the treatment of choice;
- Forced manual removal – almost universally avoided due to the risk of massive haemorrhage and subsequent hysterectomy; and
- Conservative management – controversial as although it preserves future fertility, it exposes the woman to life threatening intra-abdominal infection and major bleeding.
Hysterectomy
Total abdominal hysterectomy is generally considered the treatment of choice for placenta accreta. This involves scheduled delivery of the foetus by caesarean section at 36-37 weeks provided there is foetal lung maturity. Once the foetus is delivered, no attempt is made to remove the placenta. The edges of the uterine incision are oversewn and hysterectomy performed. This will be performed by an experienced obstetric surgeon with a skilled obstetric anaesthetist. Urology and gynaecology oncology specialists should be close at hand.
Plans are made for emergency delivery should the women experience antepartum haemorrhage or go into spontaneous labour. However, emergency hysterectomy is associated with increased intraoperative blood losses and greater rates of blood transfusion.
Conservative management

In a study of 167 women from 25 University hospitals in France, conservative treatment was successful in 78.4% of cases. Spontaneous placental resorption occurred in 75% of women at a 13.5 week follow up. Surgical techniques were used to remove the retained placenta in 25% of women at a median follow up of 20 weeks. Just over 10% of women had hysterectomies performed within the first 24 hours following delivery and a further 10.8% had delayed hysterectomies.
Conservative management of placenta accreta remains highly controversial as although this technique preserves future fertility and avoids the complications of caesarean hysterectomy, it exposes the woman to potentially life threatening infection and massive haemorrhage.
References
- Oyelese Y, Smulian JC. Placenta previa, placenta accreta, and vasa previa. Obstetrics and Gynecology 2006; 107: 927-41.
- Sentihes L, Ambroselli C, Kayem G, Provansal M, Fernandez H, Perrotin F, Winer N, Pierre F, Benachi A, Dreyfus M, Bauville E, Mahieu-Caputo D, Marpeau L, Descamps P, Goffinet F, Bretelle F. Maternal outcome after conservative treatment of placenta accreta. Obstetrics and Gynecology 2010; 115: 526-34.
- Armstrong CA, Harding S, Mathews T, Dickenson JE. Is placenta accreta catching up with us? Australian and New Zealand Journal of Obstetrics and Gynaecology 2004; 44:210-3.
- Warshak CR, Eskander R, Hull AD, Scioscia AL, Mattry RF, Benirschke K, Resnik R. Accuracy of ultrasonography and magnetic resonance imaging in the diagnosis of placenta accreta. Obstetrics and Gynecology 2006; 108: 573-81.
- ACOG Committee on Obstetric Practice. ACOG Committee Opinion. Number 266, January 2002: Placenta accreta. Obstetrics and Gynecology 2002; 99:169-70.
- Ryan GL, Quinn TJ, Syrop CH, Hansen WF. Placenta accreta postpartum. The American College of Obstetricians and Gynecologists 2002; 5: 1069-72.
- Dwyer BK, Belogolovkin V, Tran L, Rao A, Carroll I, Barth R, Chitkara U. Prenatal diagnosis of placenta accreta: sonography or magnetic resonance imaging? Journal of Ultrasound Medicine 2008; 27: 1275-81.
- Oppenheimer L. SOGC clinical practice guideline. Diagnosis and management of placenta praevia. J Obstet Gynaecol Can 2007; 29: 261-73.
- Gielchinsky Y, Rojansky N, Fasouliotis SJ, Ezra Y. Placenta accreta – summary of 10 years: a survey of 310 cases. Placenta 2002; 23: 210-4.
- The Royal Australian and New Zealand College of Obstetricians and Gynaecologists. College statement C-Obs 20: Placenta Accreta. Nov 2003. Available from http://www.ranzcog.edu.au/publications/statements/C-obs20.pdf [Accessed 5th May 2010].
- Wong HS, Hutton J, Zuccollo J, Tait J, Pringle KC. The maternal outcome in placenta accreta: the significance of antenatal diagnosis and non-separation of placenta at delivery. NZ Med J 2008; 121: 30-8.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







