- Introduction to oral mucositis and nutrition
- Nutritional status
- Nutritional assessment
- Nutritional therapy for mucositis
Introduction to oral mucositis and nutrition
Oral mucositis is a condition in which an individual develops painful lesions of the mucus membranes of the mouth. It is a side effect of cancer treatment and usually increases in severity as the dose of chemotherapy or radiation therapy increases. Mucositis can have a devastating effect on a person’s nutritional status, because the oral pain associated with the condition often prevents individuals from eating solid food, and sometimes even from swallowing.
Mucositis can have a very severe impact on a patient’s ability to eat and drink. In very severe cases of mucositis, an individual’s cancer treatment must be interrupted, to allow the oral mucosa to heal and eating to recommence. In other cases a person may require parenteral or enteral nutrition. Parenteral nutrition refers to feeding which occurs through an intravenous tube, while enteral nutrition refers to feeding which occurs through a gastric tube (e.g. a tube inserted in the stomach).
Nutritional support is an essential component of cancer treatment and assists individuals to maintain their body weight. Individualised nutrition plans are usually formulated for each person receiving cancer treatment. These assess the patient’s changing nutritional needs throughout the course of treatment, and aim to assist the patients to maintain a healthy body weight, by ensuring they consume the required quantity of calories per day (either orally, enterally or parenterally).
Nutritional status
Mucositis is associated with poor nutritional status, however cancerous tumours also adversely affect an individual’s nutritional status. As a result, many individuals with cancerous tumours have already developed poor nutritional status when they are diagnosed with cancer, that is, before they commence treatment and develop mucositis.
Cancer
Poor nutritional status, which is indicated by rapid weight loss, is often one of the first symptoms of cancer and arises from a condition known as anorexia-cachexia syndrome.
Anorexia is a condition where an individual loses appetite and the desire to eat. It affects 15-25% of cancer patients. While the condition is associated with reduced nutritional intake, muscle wasting and weight loss, anorexia alone does not account for the extent of weight loss and muscle wasting seen in people with cancer. Even those who continue to consume their normal calorie requirements, may begin to lose weight and become wasted while they are affected by cancerous tumours.
Cachexia is a tumour-induced condition characterised by protein-energy malnutrition, involuntary weight loss and muscle wasting. It occurs more commonly with some, than other types of cancer. Individuals with cancers of the upper gastro-intestinal tract (treatment of which is most likely to induce mucositis) are particularly likely to experience cachexia.
The ways in which anorexia-cachexia causes malnutrition and muscle wasting relates to metabolic changes. Cancerous tumours consume glucose, amino acids and lipids, which would typically provide nutrition for the individual with cancer. Thus a person who has cancer consumes more energy when they are resting (known as basal energy expenditure) than a person who does not have cancer. As a result they will need to eat more to maintain their weight.
Anorexia-cachexia syndrome is experienced by almost all people during the advanced stages of cancer. The syndrome leads to further malnutrition and adversely affects the individual’s response to cancer treatment, their treatment outcome and their likelihood of survival. In addition to metabolic changes, cancer can also affect a person’s taste sensations and induce nausea and vomiting. These symptoms can induce or exacerbate anorexia.
Many individuals will already be in a poor nutritional state before they are diagnosed with cancer. They may have already developed cachexia and/or anorexia before their treatment commences. Estimates suggest that up to one third of people with head and neck cancers who survive treatment, were malnourished at the time their treatment commenced.
Cancer treatment

Both radiation and chemotherapy affect an individual’s nutritional status even in the absence of side effects which inhibit eating. However, radiation and chemotherapy are also likely to induce side effects (e.g. mucositis) which inhibit an individual’s nutritional intake, and worsen weight loss and malnutrition. Treatment for head and neck cancer can have particularly profound effects on an individual’s nutritional status. The treatment for these cancers is focused in the upper gastro-intestinal tract and so is particularly likely to induce symptoms which affect the gastro-intestinal organs, such as mucositis.
Mucositis
Mucositis is one of the most frequent and troublesome side effects of chemo and radiation therapy and can cause severe pain in the mouth. This in turn can cause or worsen malnutrition. The associations between mucositis and an individual’s nutritional status are multi-directional. The painful oral lesions which characterise mucositis make it difficult for an individual to eat and drink, and thus often reduce their overall energy intake and interest in eating food. While mucositis induces poor nutrition, good nutrition on the other hand, has been shown to improve the symptoms of mucositis and reduce the toxicity of treatment.
When mucositis symptoms improve, individuals with the condition increase nutritional intake. Until recently, improving symptoms has been difficult, because no effective treatments for the disease were available.
The adverse nutritional impact of mucositis, as well as its broader adverse effects on health and quality of life, have received increasing recognition in recent years, and new mucositis treatments, are becoming available. For example antioxidant therapies, glutamine therapy and a recently approved muco-adherent gel (Gelclair) which forms a protective barrier around the oral mucosa. These offer new treatment options which may reduce oral pain and assist an individual with mucositis to eat.
Nutritional assessment
When is nutritional assessment performed?

Individuals usually have their nutritional status assessed before they commence cancer therapy and for the duration of the cancer treatment. These regular assessments are very important as the metabolic changes which accompany tumour growth or the onset of cachexia (outlined above), sometimes mean that individuals who appear to be, or think they are eating an adequate diet, are in fact under-nourished. This is particularly true for individuals with cancers of the head and neck, who are also at greatest risk of mucositis.
Nutritional screening
There are a number of screening questionnaires which health professionals use to assess the nutritional status of a person who has cancer. An individual will usually be asked to complete a questionnaire as part of their nutritional assessment. It is also likely that the individual’s body weight and height or other measurements will be taken as part of the nutritional status screening.
Nutritional therapy for mucositis
Nutritional therapy is an essential component of cancer treatment. As mucositis is a very common side effect of cancer treatment, many people receiving cancer therapy will develop mucositis in the course of their treatment, and individuals with mucositis are almost always receiving active cancer therapy when the condition develops. Thus, health professionals assess the likelihood of each individual developing mucositis whilst on treatment, and consider this when developing a strategy for nutrition therapy.
Nutrition therapy aims to maintain the weight and health status of individuals who are well nourished at the commencement of treatment, and reverse any weight loss or nutrient deficiencies in individuals who were already under-nourished when they began treatment. It also aims to prevent further weight and health loss in this group. In doing so, nutritional therapy should optimise an individual’s treatment and recovery outcomes, and improve their quality of life during treatment. Aggressive nutrition therapy has proven effective for either stabilising or reversing weight loss in 50-88% of individuals being treated for cancer.
Nutrition therapy usually begins prior to treatment, although in the initial stages such therapy might simply involve health professionals counselling individuals about the likely nutritional side effects of the treatment and the importance of consuming sufficient nutrients. Therapy typically continues throughout cancer treatment and may be intensified (e.g. a special diet may be recommended or a feeding tube may be used) as the treatment dose increases. It is not uncommon for nutritional therapy to continue for a minimum of one year (and up to three years) after the completion of treatment.
Nutrition therapy should always be given according to an individualised plan which is flexible and prepared with the support of a dietitian who specialises in nutrition for people with cancer. Unproven or alternative therapies, which individuals may have read about in magazines or on the internet, should only be used if they are recommended by an accredited dietitian and the knowledge of their specialist.
Individuals with mucositis should be treated according to the same nutritional guidelines as other patients without mucositis, however their treatment should include a specific component aimed at reducing mucositis symptoms (e.g. pain relief). People with mucositis are especially likely to experience difficulty taking food orally, and may therefore be particularly likely to need enteral (feeding via a tube inserted in the stomach) or parenteral (feeding through an intravenous drip) nutritional support, in addition to or instead of oral nutrition therapy.
Oral nutrition
Oral nutrition interventions are all those which encourage greater oral nutrient intake, including through nutritional supplements and high-calorie or high-protein nutritional formulations. Oral feeding is the preferred method (as opposed to enteral or parenteral feeding) and health professionals will recommend oral nutrition whenever possible. Maintaining a well balanced diet in the general sense (e.g. eating a range of food from a variety of food sources and food groups) is important. However, dietary modifications (e.g. increased intake of protein or particular micronutrients) will usually be necessary to ensure a patient maintains their weight.
Many individuals will find consuming adequate nutrition orally difficult and may need the assistance of a health professional to help them plan their meals appropriately. Dieticians and others can help individuals receiving cancer treatment to plan their meals to ensure they are eating enough. An individual with mucositis will usually be encouraged to eat frequently (up to 6 times daily), protein, energy and micronutrient rich meals to ensure they do not lose weight. They may also take appetite enhancing formulations, so that they feel hungry more often, in the hope that this will cause them to eat more.
Individuals with mucositis will benefit from a carefully selected diet, containing soft foods which are easy to chew and swallow and which will not irritate the oral mucosa. The following tips may help individuals select appropriate foods:
- Eat soft foods: eat soft foods and cook vegetables and other food until soft and tender. Soft fruits such as banana, berries and watermelon can be eaten raw. Stone fruits, apples and other fruits can be stewed. Other foods which may be easier for individuals with Mucositis to eat include custard, pudding, mashed vegetables, cooked cereal such as oats and scrambled eggs. Coarse food, for example meat, can be minced.
- Fluid intake: fluids should be taken through a straw as this reduces irritation in the mouth. High-energy, nutritious drinks such as milk or liquid nutritional supplements can be taken in between or with meals. Individuals may also increase their fluid intake by adding gravy or broth to their meals.
- Avoid irritating food: many foods can further irritate the oral mucosa, particularly those which are spicy, acidic or salty. Dry and coarse food, for example raw vegetables and crackers, should also be avoided.
- Avoid hot food: hot food can also irritate the mouth and individuals with mucositis should eat foods cold or at room temperature.
- Use ice: ice or ice blocks may help to numb to mouth.
- Cut food into small pieces.
Parenteral and enteral nutrition
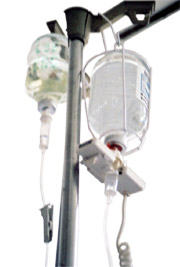
Who should receive enteral nutrition
Enteral feeding is used to assist individuals who have proper digestive functions but are unable to consume sufficient nutrients orally. This may be particularly likely in cases where mucositis (or other treatment side effects) become so severe that they endanger the individual’s treatment. An enteral tube is preferable to a parenteral tube as the gastro-intestinal organs continue to work to digest food during enteral feeding. In addition enteral feeding enables nutrients to be absorbed more efficiently than parenteral feeding and is more cost effective. An enteral tube also involves less risk of infection and is easier to administer than parenteral feeding.
Who cannot receive enteral nutrition
Enteral feeding is contraindicated in some patients, including those with the following conditions:
- Malfunctioning gastro-intestinal tract (digestive system);
- Mal-absorptive conditions;
- Obstructions in the gastro-intestinal tract which prevent food from being swallowed or digested;
- Severe bleeding;
- Severe diarrhoea;
- Severe vomiting;
- Conditions which prevent the enteral feeding tube from being inserted;
- Inflammatory bowel conditions.
Enteral nutrition strategy
An enteral nutrition tube can be placed at a number of points in the gastro-intestinal tract. The best place for the tube will be determined by a health professional, and will depend mainly on the length of time for which it is expected that enteral feeding will be required (i.e. more or less than two weeks).
There are numerous methods of administering enteral feeding solutions, for example a pump might be used to propel the feeding solution into the tube at regular intervals throughout the day, or nutrients may be continuously fed into the tube. The energy value of the feeding solution (measured in calories) will depend on the individual’s nutritional requirements and the method of feeding used (e.g. continuous, regular intervals).
There are a range of nutritional formulas which can be given via an enteral tube, and formulas containing all the nutrients typically required by individuals receiving cancer treatment have been developed. Formulas which add particular dietary nutrients (e.g. protein, fat, fibre, glutamine) are also available, and these may be added to the standard feeding formula for individuals who have deficiencies in particular nutrients.
Who should receive parenteral nutrition

- Severe mucositis;
- Intractable nausea or vomiting;
- Obstructions of the gastro-intestinal tract;
- Short bowel syndrome; and
- Ileus.
Who cannot receive parenteral nutrition
Parenteral feeding should not be used for individuals:
- Who have a functioning gut;
- In whom intravenous access cannot be gained;
- Who need nutritional support for <5 days; and
- Who are not expected to live more than six months.
Parenteral nutrition strategy
Parenteral nutrition is administered via an intravenous drip, and therefore a catheter through which the feeding formula can be administered, must be inserted if it is not already in place. Parenteral feeding solutions should be tailored to the needs of the individual. They typically contain amino acids, dextrose, lipids, vitamins, minerals and trace elements, fluids and electrolytes. Some may also contain insulin, heparin and antacids.
Parenteral and enteral nutrition at home
Both enteral and parenteral feeding formulas can be administered at home, so that individuals are not prevented from leaving hospital because of parenteral or enteral feeding. Health professionals will teach individuals receiving such nutritional support, and their carers, how to administer the nutritional formulas and take care of the feeding tube or catheter, so that it does not become infected. Individuals receiving enteral or parenteral nutrition therapy at home must have a safe and clean home environment and they must continue to visit a hospital or clinic for medical check-ups.
Withdrawing parenteral nutrition
Parenteral nutrition cannot be abruptly discontinued. It must be gradually reduced, while oral or enteral feeding is re-introduced. When an individual is able to tolerate consuming 50% of their nutritional requirements enterally or consuming a full liquid diet (i.e. all their nutritional requirements orally, but in liquid rather than solid forms), parenteral therapy can be halved. When an individual is able to consume 75% of their nutritional requirements on enteral therapy or are able to eat solid foods in addition to the liquid diet, parenteral nutrition can be withdrawn completely
Special considerations
Religious beliefs
Some individuals may undergo periodic fasting as part of their religious customs. Waiving any religious customs which restrict nutritional intake during cancer treatment is essential for ensuring the treatment is as effective as possible. Individuals who usually observe periods of fasting for religious purposes should inform their doctor and consult relevant religious leaders about waiving dietary restrictions for the treatment period.
More information
 |
For more information on oral mucositis, including treatments and some useful videos, see Mucositis. |
 |
For more information on nutrition, including information on types and composition of food, nutrition and people, conditions related to nutrition, and diets and recipes, as well as some useful videos and tools, see Nutrition. |
References
- Nutrition in cancer care [online]. Bethesda, MD: National Cancer Institute. 11 August 2009 [cited 20 September 2009]. Available from: [URL]
- Cheng KKF, Leung SF, Liang RHS, et al. A patient-reported outcome instrument to assess the impact of oropharyngeal mucositis on health-related quality of life: A longitudinal psychometric evaluation. Support Care Cancer. 2009; 17(4); 389-98.
- Hartvig P, Honoré E. Supportive care: Nutrition problems, alopecia and mucositis. Eur J Oncol Pharm. 2008; 2(1): 26-7.
- Kiyomoto D. Head and neck cancer patients treated with chemo-radiotherapy require individualized oncology nutrition. J Am Diet Assoc. 2007; 107(3): 412-5.
- Beck SL, Cella D. Advancing the assessment and treatment of mucositis [online]. Proceedings of the Oncological Nursing Society 29th Annual Congress. 19 October 2004 [cited 30 September 2009]; 39-40. Available from: [URL]
- Gelclair Frequently Asked Questions [online]. Helsinn Healthcare SA Switzerland. 20 September 2007 [cited 19September 2009]. Available from: [URL]
- Dempsey DT, Mullen JL. Prognostic value of nutritional indices. J Parenter Enteral Nutr. 1987; 11(5 Suppl): 109-14S.
- Bauer J, Capra S, Ferguson M. Use of the scored Patient-Generated Subjective Global Assessment (PG-SGA) as a nutrition assessment tool in patients with cancer. Eur J Clin Nutr. 2002; 56(8): 779-85.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.








