
- What is intracytoplasmic sperm injection?
- History of intracytoplasmic sperm injection
- Effectiveness of intracytoplasmic sperm injection
- Indications for intracytoplasmic sperm injection
- How is intracytoplasmic sperm injection performed?
- Benefits of intracytoplasmic sperm injection
- Limitations of and risks associated with intracytoplasmic sperm injection
- Psychological aspects of intracytoplasmic sperm injection
What is intracytoplasmic sperm injection?
Intracytoplasmic sperm injection is a micromanipulation technique used in the process of in vitro fertilisation (IVF). It involves injecting a single sperm into the centre of a mature oocyte under a microscope (i.e. injecting the sperm through the egg’s shell so that the sperm does not need to penetrate the shell in order to fertilise the egg).
The injected ovum is them monitored in the lab for signs of fertilisation. The injection of sperm directly into the centre of ovum bypasses a number of events in the fertilisation process, which are highly dependent on the ability of the sperm to travel to the site of an egg, and then recognise, bind to, penetrate and fertilise that egg. This technique is therefore used to treat male factor infertility related to the quality and quantity of sperm.
The natural fertilisation of an egg by sperm is highly dependent on the motility of sperm. In men with low sperm count or morphologically abnormal sperm, the number of sperm which have the ability to travel to and fertilise an egg is reduced. Because of this, many men with a low sperm count or morphologically abnormal sperm are infertile.
Traditional IVF techniques have also been highly dependent on sperm motility. For example the most popular technique for IVF is known as the ‘swim up’ in which sperm and eggs are placed in a culture which mimics conditions inside the uterus and the sperm then recognise and bind to the eggs as they swim around. Historically this meant that IVF was not a particularly effective treatment for male factor infertility related to semen quality. The development of intracytoplasmic sperm injection techniques have revolutionised the treatment of male factor infertility. They have a high rate of success for treating men with low sperm counts or morphologically abnormal sperm.
History of intracytoplasmic sperm injection
Monash scientists demonstrated the world’s first micro injection technique using eggs and sperm of mice in 1987. While this technique was relatively efficient for fertilising mice eggs, much lower rates of fertilisation occurred when the technique was applied to humans. This is because of differences in reproductive functions between the two mammals. In practice subzonal microinjection of human eggs had a low rate of success.
On the contrary, intracytoplasmic sperm injection showed relatively low success in animal studies, but have proven extremely efficacious in assisting human reproduction.
Subzonal microinjection was superseded by intracytoplasmic sperm injection, a vastly more effective technique, in the early 1990s. The first live birth resulting from this procedure occurred in 1992, from an embryo conceived by a group of Belgian scientists. Intracytoplasmic sperm injection has since revolutionised the treatment of infertility related to abnormal semen parameters, which were generally not effectively treated with traditional IVF techniques.
The use of intracytoplasmic sperm injection has increased dramatically as it is a highly successful treatment for male factor infertility. For example in Australia, intracytoplasmic sperm injection now accounts for more treatment cycles than traditional IVF techniques, and the number of intracytoplasmic sperm injection procedures performed annually increased from around 2000 in 1994, to more than 8000 in 2003. In the US, the proportion of IVF treatments involving intracytoplasmic sperm injection increased from 11% in 1995 to 57.5% in 2004.
Effectiveness of intracytoplasmic sperm injection
In Australia and New Zealand, 21.2% of treatment cycles started for intracytoplasmic sperm injection resulted in live birth, the same proportion as for traditional IVF.
Indications for intracytoplasmic sperm injection
Intracytoplasmic sperm injection is indicated when infertility is underpinned by male factors relating to abnormal semen parameters. There is no evidence that intracytoplasmic sperm injection is more effective than other IVF techniques when other factors underlie a couples’ infertility.
How is intracytoplasmic sperm injection performed?
A single viable sperm and oocyte are then selected for injection. Microscopic instruments (a holding pipette and an injecting pipette) are used to pick up the sperm and inject it into the centre of the ovum. The pipette is then removed and the injected ovum placed in a growth culture medium, where, if the procedure has been successful, fertilisation will occur, usually 16-20 hours following the injection.
Successfully fertilised embryos will then be implanted into a woman’s uterus,or cryopreserved for future use.
Retrieved spermatozoon and oocytes must be cleaned prior to use and then examined under a microscope so that the most appropriate gametes can be selected for the injection process.
The spermatozoon chosen for injection should preferably be motile and display no morphological abnormalities. However intracytoplasmic sperm injection is used to overcome severe male factor infertility, in which no motile sperm are available. It is thus not dependent on the selection of motile sperm, however fertilisation rates are much lower when immotile sperm are used. If sperm retrieved using an ejaculation technique (e.g. masturbation) are all immotile a doctor may attempt to retrieve sperm from the testicles or epidymal tube. These sperm have been shown to result in higher fertilisation rates even if they are immotile, compared to ejaculated sperm. Sperm suspensions are commonly diluted using chemicals so that the sperm move more freely and are easier to manipulate under a microscope.
Once the sperm and oocytes are prepared, the injection process can begin. The injection process requires two microsurgical instruments. A standard holding pipette is used to manipulate the ovum throughout the procedure. A bevelled, sharpened injection pipette is used to retrieve spermatozoon from their suspension and inject them into the oocytes. The selected spermatozoon is retrieved from the suspension tail first. The scientist manipulating the sperm will line the pipette up with the tail of the selected sperm and then draw it into the pipette. Drawing the tail into the pipette first means that the sperm will be injected into the egg head first.
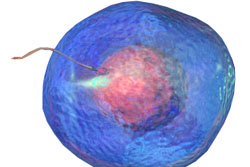 |
|
Image courtesy of Blausen Medical Communications. Contact Andrew Walbank. |
The sperm must then be injected into the ovum. The injecting pipette is advanced gently into the egg and through the zona pellucida and to the plasma membrane which protects the nucleus (i.e. the centre) of the ovum. The plasma membrane often breaks spontaneously, however if this does not occur, the scientist performing the micromanipulation can gently rupture the membrane using the injection pipette. Fluid will flow back into the injection pipette once the plasma membrane is ruptured, after which the sperm is carefully expelled into the ovum and the pipette withdrawn, completing the procedure.
The injected ovum is then cultured for 16-20 hours, after which fertilisation is assessed. Oocytes which have fertilised normally are separated from abnormal fertilisations and unfertilised oocytes.
Normally fertilised oocytes are placed in a fresh medium design to facilitate their growth, while unfertilised oocytes may remain in the insemination medium for possible late fertilisation. The fertilised embryos will then be grown for a period of 2-5 days, until they have grown sufficiently (i.e. to a size of eight cells or more) for implantation or Cryopreservation.
Benefits of intracytoplasmic sperm injection
Before the development of intracytoplasmic sperm injection, male infertility related to abnormal semen count was considered largely untreatable. This assisted reproductive technique has therefore enabled many couples who would not previously have been able to conceive, or who would have been reliant on donor sperm, to conceive a biological child.
Limitations of and risks associated with intracytoplasmic sperm injection
There are a number of risks and limitations associated with intracytoplasmic sperm injection. In particular, as the techniques are relatively new (i.e. the first intracytoplasmic sperm injection babies are not yet 15 years old), the long term effects of intracytoplasmic sperm injection on the health of the individuals conceived is largely unknown.
The second main concern about intracytoplasmic sperm injection is that babies born as a result of this procedure will be more likely to have congenital abnormalities than babies conceived naturally. This concern arises because intracytoplasmic sperm injection babies are often conceived using morphologically abnormal sperm, including sperm with chromosomal and genetic abnormalities. Because male babies inherit the genetic make up of their father’s sperm, there is an increased chance in male intracytoplasmic sperm injection babies having these abnormalities. For example when sperm with abnormal Y chromosomes are used for intracytoplasmic sperm injection conception, the genetic make up of the Y chromosome is inherited by any male offspring born from that conception. In the absence of intracytoplasmic sperm injection, men with Y chromosome abnormalities would be unable to conceive and thus unable to pass down their genetic abnormalities. As such the fertility problems overcome using intracytoplasmic sperm injection may be passed on to the next generation. This, at least in theory, has the potential to contribute to an overall decline in male fertility over time.
Psychological aspects of intracytoplasmic sperm injection

Couples should also be aware that intracytoplasmic sperm injection may fail, and be encouraged to discuss alternative options (e.g. use of donor sperm, adoption). In addition, couples undergoing intracytoplasmic sperm injection should be aware of and discuss the increased risk of congenital abnormalities, particularly in male offspring.
More information
 |
For more information on infertility, including investigations and treatments, as well as some useful animations, see Infertility. |
 |
For more information on alternative treatments, see Infertility Treatments / Assisted Reproductive Technologies (ARTs). |
References
- Malter, H.E. Cohen, J. Intracytoplasmic Sperm Injection: Technical Aspects, World Health Organisation, available from: www.who.int/reproductive-health/infertility/15.pdf
- Gianaroli, L. Plachot, M. van Kooij, R. et al, "ESHRE guidelines for good practice in IVF laboratories" in Human Reprod, 2000, 15 (10):2241-46.
- Hirsch, A. "Male Subfertility [Clinical Review]" in BMJ, 2003, 327:669-672.
- Balen, A.H. Rutherford, A.J. "Management of Infertility: Clinical Review" in BMJ, 2007, 335:608-11.
- Cohen, J. Troussen, A. Dawson, K. et al, "The Early Days of IVF outside the UK" in Hum Reprod. Update, 2005, 11(5):439-60.
- Palermo, G., Joris, H., Devroey, P. Van Steirteghem, A.C. "Pregnancies after intracytoplasmic sperm injection of single spermatozoon into an oocyte" in Lancet, 340:17-18.
- Jain, T. Gupta, R.S. "Trends in the use of intracytoplasmic sperm injection in the United States" in NEJM, 2007, 357:251-7.
- Waters, A. Dean, J.H. Sullivan, E.A. Assisted Reproduction Technology in Australia and New Zealand 2003, Australian Institute for Health and Welfare, National Perinatal Statistics Unit, available from: www.npsu.unsw.edu.au/NPSUweb.nsf/page/art9high
- Royal College of Obstetricians and Gynaecologists. Fertility: Assessment and treatment for people with fertility problems – Clinical Guideline [online]. Royal College of Obstetricians and Gynaecologists, 2004 [cited 30 October 2008]. Available from URL: http://www.rcog.org.uk/womens-health/clinical-guidance/fertility-assessment-and-treatment-people-fertility-problems
- van Rumste, M.M. Evers, J.L. Farquar, C.M., "ICSI versus conventional techniques for oocyte insemination during IVF in patients with non-male factor subfertility: a Cochrane review" in Cochrane Database of Systematic Reviews 2003, Issue 2. Art. No.: CD001301.
- Kurinczuk, J.J. Bower, C. "Birth Defects in Infants Conceived by intracytoplasmic sperm injection: an alternative interpretation" in BMJ, 1997, 315:1260-65.
- Bonduelle M, Legein J, Buysse A, Van Assche E, Wisanto A, Devroey P, et al. "Prospective follow-up study of 423 children born after intracytoplasmic sperm injection" in Hum Reprod 1996;11:1558-64.
- Faddy, M.J. Silber, S.J. Gosden, R.J. "Intracytoplasmic Sperm Injection and Infertility" in Nature Genet, 2001, 29:131.
- National Health and Medical Council of Australia, Ethical Guidelines on the use of assisted reproductive technology in clinical practice and research, National Health and Medical Council of Australia, available from: www.nhmrc.gov.au/publications/synopses/e78syn.htm
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







