- What is Idiopathic Subglottic Stenosis (ISS) (Idiopathic laryngotracheal stenosis (ILTS)) (Idiopathic tracheal stenosis)?
- Statistics
- Risk Factors
- Progression
- Symptoms
- Clinical Examination
- How is it Diagnosed
- Prognosis
- Treatment
- References
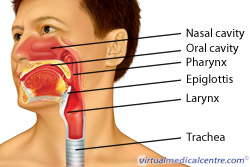
What is Idiopathic Subglottic Stenosis (ISS) (Idiopathic laryngotracheal stenosis (ILTS)) (Idiopathic tracheal stenosis)?
Idiopathic subglottic stenosis (ISS) is narrowing of the upper airway caused by inflammation and scar tissue, due to an unknown cause.
Idiopathic means that something has an unknown cause. Subglottic refers to the area of the airway that is narrowed (under the vocal cords, or ‘glottis’). Stenosis means a narrowing.
Many things can cause the airway to narrow. ISS will not be diagnosed if another cause is found for the narrowed airway (as diagnosis of ISS requires the narrowing to be from an unknown cause). Known causes of narrowed airway include:
- Mechanical trauma, for example due to intubation, where a tube is put down someone’s throat to help them breathe (the most common cause);
- Granulomatosis with polyangiitis (formerly known as Wegener’s granulomatosis), which is an inflammatory condition;
- External trauma;
- burns due to inhaled hot air, and irradiation;
- Collagen vascular diseases, including polyarteritis, scleroderma and sarcoid;
- Amyloid disease;
- Surgery;
- Upper respiratory infections, including bacterial tracheitis, tuberculosis, diphtheria and histoplasmosis; and
- Congenital stenosis (the person is born with it).
Statistics

Risk Factors
The cause of ISS is unknown. It is unclear why it almost always affects women, and although it has been suggested that hormones are involved, this has not been proven.
It has been suggested that Gastro-oesophageal reflux disease both causes ISS, and makes it worse, though again this has not been proven.
A recent theory is that a severe coughing episode causes microscopic trauma and scarring in the trachea (windpipe), which causes it to narrow.
Progression
It is not clear how ISS progresses. Most authors believe it gradually gets worse over time. Symptoms of ISS, such as shortness of breath when exercising, may get worse over months or years and develop into shortness of breath at rest, noisy breathing and chronic cough. ISS commonly reoccurs after treatment, especially non surgical treatment. Due to the slow progression of symptoms, people with ISS are often misdiagnosed as having asthma and treated for that instead.
Symptoms

These symptoms may be caused by other conditions (such as asthma or COPD) more commonly than they are caused by ISS. A clear description of when symptoms occur, how long they have lasted for, and what makes symptoms better or worse will be helpful to the doctor in making a diagnosis. People who experience serious symptoms such as coughing blood and severe shortness of breath should seek immediate medical attention.
Clinical Examination
People with ISS tend to be otherwise healthy. For this reason and due to the gradual onset of symptoms, it is not uncommon for ISS to be initially diagnosed and managed as asthma. There is usually little for a doctor to see upon clinical examination, although if stenosis is severe they may detect noisy breathing.
How is it Diagnosed

Firstly, tests to rule out other causes are carried out, including:
- CT scan;
- chest x-ray;
- respiratory function studies; and
- a blood test (to rule out Granulomatosis with polyangiitis (formerly known as Wegener’s granulomatosis) – an inflammatory condition that will not be cured with surgery for ISS).
Once these tests have been carried out, then a laryngo-tracheo-bronchoscopy (a form of endoscopy) may be carried out. This is where the doctor looks down the throat into the lungs with a tiny camera under local anaesthetic, usually with some sedation. This test is used to determine how large the area of narrowing is, how the vocal cords are moving, and the state of the airway. During the endoscopy, biopsy specimens from the area of narrowing may be taken. Digital photography may also be carried out to measure how severe the stenosis is.
Prognosis
People with ISS are thought to do better with treatment if the area of scar tissue in their windpipe is short (less than 1cm) and the scar tissue is soft.
Different studies report different success rates with treatments, but in general:
- Short areas of scar tissue may not require procedures to fix them, or if they do, may only require 1-2 procedures.
- Long areas of scar tissue tend to recur after procedures such as dilation and laser treatment, often around 6-9 months following surgery.
- Some studies report up to 90% of patients have good to excellent long term results after surgery for ISS.
- Long term problems that may occur after surgery for ISS include changes in voice quality such as difficulty with loud speaking and singing and the need for repeat procedures because symptoms have returned.
Treatment
Conservative management and medications
Observation
If symptoms are absent or mild, so that the ISS does not affect quality of life or limit function, the most appropriate course of action may be to monitor the condition.
Treatment of reflux
If a patient has symptoms of reflux, some doctors suggest anti-reflux medication should be started and the resulting improvement in symptoms monitored over a period of 3 months before considering a surgical procedure.This approach is controversial, as not all doctors believe treating reflux will improve ISS;
Steroid injections
Steroid injections into the area of narrowing have been used in the past to prevent stenosis reoccurring following surgery. There has been no clear evidence to support this practice, so it has been abandoned.
Mitomycin-C
Mitomycin-C is a drug that may be applied to the narrowed airway at the time of surgery to prevent the stenosis reoccurring. Mitomycin-C may delay the stenosis reoccurring, rather than prevent it.
Procedures and surgery
Airway dilation
Laser
Laser may be used to cut and widen the narrowed airway. This is done using endoscopy. It may be used with or without mitomycin-C. Around 60% of patients require a further procedure after this technique, with the average length between procedures being 9 months;
Open surgery
Open surgery may be used to cut out the affected part of the airway and rebuild it (laryngotracheal resection and reconstruction). This treatment is successful in restoring the airway whilst preserving voice quality in over 90% of patients. Reconstructive procedures may involve putting extra cartilage into the airway to widen the narrow area (cartilage grafts) or removal of the narrowed area, then reattaching the two ends (segmental resection). Due to the success of these reconstructive procedures, it has been suggested that these may be a suitable initial treatment option for ISS.However, surgery on the airway has greater risks than other procedures, so some doctors think it is better to use it if other treatments fail. Surgery is most helpful if the scarred, narrowed area is long and complex, as this is more difficult to fix with other treatments;
Tracheostomy
Tracheostomy, where a hole is cut in the front of the neck to create an opening into the windpipe, is now rarely required. Tracheostomies may increase the area of damaged windpipe (trachea), which can complicate eventual repair.
References
- Damrose E. On the development of idiopathic subglottic stenosis. Medical Hypotheses. 2008;71:122-5.
- Valdez T, Shapshay S. Ideopathic Subglottic stenosis revisited. Annal Oto Rhino Laryng 2002;111:690-5.
- Harries P et al. Idiopathic tracheal stenosis. The Journal of Laryngology and Otology. 1996; 110: 973-5.
- Park S, Streitz J, Rebeiz E, Sbapshay S. Idiopathic subglottic stenosis. Arch Otolaryngol Head Neck Surg. 1995; 121: 894-7.
- Loutsidis A et al. Surgical management of idiopathic subglottic tracheal stenosis. European Journal of Cardio-thoracic Surgery. 2000; 17: 488-91.
- Dedo HH, Catten MD. Idiopathic progressive subglottic stenosis: finding and treatment in 52 patients. Ann Otol Rhinol Laryngol. 2000; 110: 305-11.
- Giudice M et al. Idiopathic subglottic stenosis: management by endoscopic and open-neck surgery in a series of 30 patients. Eur Arch Otorhinolaryngol. 2003; 260: 235-8.
- Ashiku SK, Kuzucu A, Grillo HC, et al. Idiopathic laryngotracheal stenosis: effective definitive treatment with laryngotracheal resection. J Thorac Cardiovasc Surg. 2004; 127: 99-107.
- Prakash U. Uncommon Causes of Cough: ACCP Evidence-Based Clinical Practice Guidelines. Chest. 2006;129;206S-19S.
- Lorenz R. Adult laryngotracheal stenosis: etiology and surgical management. Curr Opin Otolaryngol Head Neck Surg 2003; 11: 467-72.
- Yamada S, Kikuchi K, Kosaka A, Inoue H, Umemura S. Surgical management of idiopathic tracheal stenosis. Japanese Journal of Thoracic & Cardiovascular Surgery. 1999; 47(7): 335-8.
- Brandenburg JH. Idiopathic subglottic stenosis. Transactions – American Academy of Ophthalmology & Otolaryngology. 1972; 76(5): 1402-6.
- Grillo H, Mark C, Mathisen D, Wain J. Idiopathic larygotracheal stenosis and its management. Annals Thoracic Surgery. 1993;56:80-7.
- Beddow E, Rice A, Sheppard M, Goldstraw P. Idiopathic tracheal and bronchial stenosis in two pediatric patients. Annals of Thoracic Surgery. 2004; 77(5): 1829-32.
- Bodart E, Remacle M, Lawson G, Mayne A, Vandenbossche P. Idiopathic subglottic stenosis in a nine-year-old boy: diagnosis and management. Pediatric Pulmonology. 1998; 25(2): 136-8.
- Mark EJ et al. Idiopathic Tracheal Stenosis: A Clinicopathologic Study of 63 Cases and Comparison of the Pathology with Chondromalacia. Am J Surg Pathol 2008; 32: 1138-43.
- Benjamin B, Jacobson I, Eckstein R. Idiopathic subglottic stenosis: diagnosis and endoscopic laser treatment. Annal Otol Rhinol Larygol. 1997:106:770-4.
- Roediger F, Orloff L, Courey M. Adult Subglottic Stenosis: Management with Laser Incisions and Mitomycin-C. Laryngoscope. 2008; 118: 1542-6.
- Maronian N, Azadeh H, Waugh P, Hillel A. Association of laryngopharyngeal reflux disease and subglottic stenosis. Ann Otol Rhinol Laryngol 2001; 110: 606-12.
- Terra RM. de Medeiros IL. Minamoto H. Nasi A. Pego-Fernandes PM. Jatene FB. Idiopathic tracheal stenosis: successful outcome with antigastroesophageal reflux disease therapy. Annals of Thoracic Surgery. 2008; 85(4): 1438-9.
- Bhalla M. Grillo HC. McLoud TC. Shepard JO. Weber AL. Mark EJ. Idiopathic laryngotracheal stenosis: radiologic findings. American Journal of Roentgenology. 1993; 161(3): 515-7.
- Andrilli A et al. Long-term results of laryngotracheal resection for benign stenosis. European Journal of Cardio-thoracic Surgery. 2008; 33: 440-3.
- Perepelitsyn I, Shapshay SM. Endoscopic treatment of laryngeal and tracheal stenosis- has mitomycin C improved the outcome? Otolaryngol Head Neck Surg 2004; 131: 16-20.
- Smith M, Elstad M. Mitomycin C and the endoscopic treatment of laryngotracheal stenosis: are two applications better than one? Laryngoscope. 2009; 119(2): 272-83.
- Lee K, Rutter M. Role of Balloon Dilation in the Management of Adult Idiopathic Subglottic Stenosis. Annals of Otology, Rhinology, and Larygology. 2008; 7(2): 8l-4.
- Simpson G, Strong M, Healy G, Shapshay S, Vaughan C. Predictive factors of success or failure in the endoscopic management of laryngeal and tracheal stenosis. Ann Otol Rhinol Laryngol 1982; 91: 384-8.
- Herrington H et al. Modern Management of Laryngotracheal Stenosis. Laryngoscope. 2006; 116: 1553-7.
- Chandran S, Sataloff R. Idiopathic tracheal stenosis. Ear, nose and throat Journal. 2009; 88(4): 860-1.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.