- What is Heart Failure
- Statistics on Heart Failure
- Risk Factors for Heart Failure
- Progression of Heart Failure
- Symptoms of Heart Failure
- Clinical Examination of Heart Failure
- How is Heart Failure Diagnosed?
- Prognosis of Heart Failure
- How is Heart Failure Treated?
- Heart Failure References
What is Heart Failure
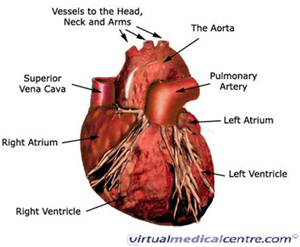
Heart failure, in simple terms, is when the heart fails to maintain an adequate circulation of blood around the body, owing to a defect in the heart’s pumping action. Heart disease can lead to heart failure.
Statistics on Heart Failure
It is estimated at least 300,000 Australians currently suffer heart failure and around 30,000 new cases of heart failure are diagnosed each year:
- Heart failure is generally a disease affecting the older generation: 13% of people aged 65 and over see their GP for heart failure.
- In 1996 and 1997, 41,000 hospitalisations reported heart failure as a principal diagnosis.
- During 1996 and 1997, heart failure contributed to 2% of all deaths;
- Heart failure is estimated to account for $411 million of the total direct health costs attributed to cardiovascular disease (estimated in 1993-94 at $3,719 million). This figure for heart failure includes $140 million per year on hospitalisation and $135 million per year on nursing home costs.
Heart failure is the only major cardiovascular disease that still has an increasing number of cases in regions worldwide:
- 20 per 1,000 people have heart failure, rising to as many as 130 per 1,000 for those aged over 65 years.
- In Western Europe there are over five million heart failure patients.
- 2-3 new cases of heart failure per 1,000 people are reported in Europe every year.
- In the USA there are around five million heart failure sufferers, with 400,000 new cases diagnosed each year.
- Worldwide among the 70-80 age group, 100 in every 1,000 people have heart failure.
The incidence and prevalence of heart failure is still rising and it is predicted that this will continue. There are two main reasons for this increase.
Advances of modern medicine
Improved management of cardiovascular disease means that patients survive longer. Many patients who have heart attacks now survive because of modern medical treatment and faster response times from medical services. However, the heart muscles of these patients are often damaged and can no longer compensate, leading to the development of heart failure. This has been described as an “ironic failure of success”.
Ageing of the population
More older people have heart failure than younger people, which may be due to the greater frequency of common risk factors for heart failure (e.g. high blood pressure, heart attack and diabetes mellitus. One in ten people over 80 years old have heart failure. In Europe, the average age of the population in 1950 was 29.2 years; by 1998 this had risen to 37.1 years. By 2050, the average age of the population is predicted to reach 47.7 years, leading to yet higher rates of heart failure.
Risk Factors for Heart Failure
- Infection
- Anaemia
- Thyrotoxicosis
- Pregnancy:Women with rheumatic valvular disease can first experience symptoms during pregnancy; following delivery of the baby, these symptoms may be resolved.
- Abnormal heart rhythms
- Rheumatic fever
- Infective endocarditis and myocarditis
- High blood pressure
- Heart attack
- Pulmonary embolism
- Over-exercise
- Sudden increase in salt in the diet
- Excessive environmental heat or humidity
- Emotional crises
Progression of Heart Failure
Heart failure can occur when the heart has been overworked or damaged in some way. High blood pressure over many years, heart valve disease, defects in the heart at birth and infection are some of the causes.
The most common cause is a heart attack – also known as myocardial infarction or “coronary”. Heart failure can result from one large heart attack or several smaller ones.
Another common cause is a disease of the heart muscle known as cardiomyopathy. This can be caused a viral infection or excess alcohol consumption on a regular basis.
The cost and burden of heart failure is expected to increase markedly due to a number of factors:
- The ageing population
- The projected increase in the number of older people with coronary heart disease and high blood pressure
- The decrease in fatality rates associated with acute coronary disease
- Improved diagnosis of CHF because of the increased use of sensitive techniques such as echocardiography
How is Heart Failure Diagnosed?
- Full blood count
- Urea and electrolytes
- Thyroid function tests
- Liver function tests
- Pulse oximetry
- Electrocardiography
- Chest x-ray
Prognosis of Heart Failure
Heart failure is usually a chronic illness, and it may worsen with infection or other physical stressors. But with medication and correction of underlying disorders, it can be controlled.
How is Heart Failure Treated?
A variety of medications are used to treat heart failure in order to reduce the work the heart has to do, relieve symptoms and reduce the build-up of fluid:
- Diuretics or fluid tablets work on the kidney to remove excess fluid from the body
- ACE inhibitors relax blood vessels making it easier for the heart to pump blood to all tissues of the body
- Digoxin helps the heart beat more strongly, slowly and regularly
- Spironolactone is used in moderate and severe heart failure to reduce the impact of hormones on the heart and prevent scarring
Heart Failure References
- Albanese MC, Plewka M, et al. Use of medical resources and quality of life of patients with chronic heart failure: A prospective survey in a large Italian community hospital. European Journal of Heart Failure. 1999; 1(4): 411-7.
- American Heart Association statistical database: Economic cost of cardiovascular disease, 1999.
- Beamish RE. Heart failure: the ironic failure of success. Canadian Journal of Cardiology. 1994; 10: 603.
- Cowie MR, Mosterd A, et al. The epidemiology of heart failure. European Heart Journal 1997; 18: 208-25.
- Dominguez LJ, Parrinello G, Amato P, Licata G. Trends of congestive heart failure epidemiology: contrast with clinical trial results. Cardiologia 1999; 44: 801-8.
- Guidelines for the contemporary management of the patient with chronic heart failure in Australia. National Heart Foundation of Australia and the Cardiac Society of Australia. www.heartfoundation.com.au
- Kannel WB, Belanger AJ. Epidemiology of heart failure. American heart Journal. 1991; 121: 1042-7.
- Krum H, Tonkin AM, Currie R, et al. Frequency, awareness and pharmacological management of chronic heart failure in Australian general practice. The Cardiac Awareness Survey and Evaluation (Case) Study. Med J Aust 2001; 174: 439-44.
- Linne AB, Liedholm H, et al. Health care costs of heart failure: Results from a randomised study of patient education. European Journal of Heart Failure. 2000; 2(3): 291-7.
- McMurray JJ, Stewart S. Heart failure – epidemiology, aetiology, and prognosis of heart failure. Heart 2000; 83: 596-602.
- O’Connell JB. The Economic Burden of Herat Failure. Clinical Cardiology 2000; 23(Suppl3): 6-10.
- Stewart S, Jenkins A, Buchan S, Capewell S, McGuire A, McMurray JJV. The current cost of heart failure in the UK – an economic analysis. Eur J Heart Failure, 2002; 4: 361-71.
- Stewart S, et al. The current cost of heart failure to the National Health Service in the UK, European Journal of Heart Failure 2002; 4(3): 361-71.
- Swedberg K, Rosengren A, Schaufelberger M, et al. Presentation at ACC Annual Meeting 2003.
- United Nations Population Division, World Population Prospects: The 2002 Revision and World Urbanisation Prospects: The 2001 Revision.
- Wolinsky FC. The risk of hospitalisation for congestive heart failure among older adults. Med Care 1997; 35: 1031-43.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







