- Introduction
- How diabetes affects eye health
- Impact of vision on quality of life
- Prevention
- Treatment
Introduction
The most recent data on diabetes in Australia estimates that 898,800 Australians have been diagnosed with diabetes at some time in their lives. Of these, 87% had Type 2 diabetes (787,500 people) and 10% (87,100 people) had Type 1 diabetes.
People living with Type 1 diabetes represent 0.4% of the Australian population. The cause of Type 1 diabetes is not well understood, but is due to both genetic and environmental factors.
Type 2 diabetes is much more common than Type 1 and rates are higher in outer regional or remote areas than in cities. It is more common in men and in people over 35 years old. Rates of Type 2 diabetes are steadily increasing worldwide.
 |
For more information about the types of diabetes, lifestyle advice, treatments, videos and more, see Diabetes. |
How diabetes affects eye health
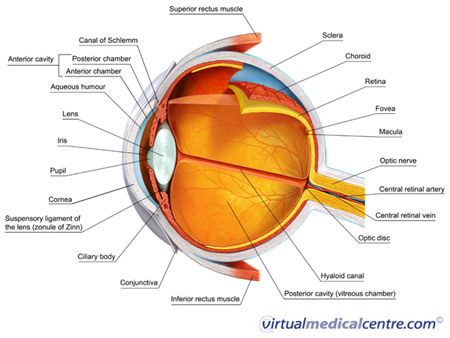
In the United States, diabetes is the leading cause of blindness between the ages of 20 and 74. This is because diabetes can damage the tiny, delicate blood vessels that supply the retina at the back of the eye. This can in turn cause damage to the cells of the retina, which are responsible for normal sight. Disrupting normal blood flow to these cells can cause permanent blindness.
Information on re-publishing of our images
This process is called diabetic retinopathy and it is a common complication of all forms of diabetes, particularly if it is not well treated and sugar levels are not well controlled. It is estimated that of all diabetics in the world, approximately one-third of them have some form of diabetic retinopathy. About 10% of diabetics have a level of diabetic retinopathy that is threatening their vision.
In the early form of diabetic retinopathy (called non-proliferative diabetic retinopathy), the blood vessels of the retina start to weaken and can bleed into the retina tissue. This can trigger swelling and damage in nearby tissues, such as the macula. The macula is the central part of the retina that provides our detailed, central vision – any damage to the macula can leave individuals with a permanent black spot in the middle of their vision. This process is called macular oedema. Macular oedema is the number one cause of loss of sight in diabetic retinopathy.
This form diabetic retinopathy can also progress to a more dangerous form, called proliferative diabetic retinopathy. In this form, not enough blood is reaching the cells of the retina and they become deprived of oxygen. In an effort to provide more oxygen, the retina starts to grow new, fragile blood vessels to reach those cells. However, these new blood vessels also have a strong tendency to rupture and bleed, causing further damage to the retina. In extreme cases, these new blood vessels can lead to retinal detachment from the inside of the eyeball altogether, causing blindness.
One of the chief problems in preventing and treating all forms diabetic retinopathy is that you may have no obvious symptoms in the early stages. Unless an eye specialist does a thorough eye examination regularly, diabetic retinopathy may be progressing without you realising it. It is therefore essential that all people with diabetes get regular screening for diabetic retinopathy done by an eye specialist.
 |
For more information about the different types of diabetic retinopathy and how they can be diagnosed and treated, see Diabetic Retinopathy. |
Impact of vision loss on quality of life

While much more research is needed in this area, vision loss due to diabetes can have a wide-ranging, permanent and profound effect on quality of life. Other areas of daily living that can be strongly affected by diabetic retinopathy include reading, driving (especially at night), working, sports, socialising and self-care. People with diabetic retinopathy have reported being much more afraid of having an accident.
Prevention
Given the terrible lifelong consequences of uncontrolled diabetic retinopathy and its effect on vision, reducing the risk or slowing the progression of the disease is essential for all people with diabetes. People with diabetes should be screened for diabetic eye disease regularly, as well as provided with the best treatment to control their blood sugar levels and blood pressure. This can reduce risk of losing vision by as much as 95%. However, people who have good control of their sugar and blood pressure may still progress to diabetic retinopathy in the long term. Vision loss can be identified early by frequent eye examinations. By treating diabetic retinopathy or macular oedema as early as possible, further progression of the disease can be prevented. Data suggests that approximately 1 in 5 Australians with diabetes are not being screened as often as is recommended by health professionals.
Eye doctors recommend eye examinations every 2 years for people with any form of diabetes. If diabetic retinopathy is diagnosed, patients should be examined even more frequently. Some people have a higher risk of progressing to diabetic retinopathy, such as Indigenous Australians, Australians with a non-English speaking background, people who have poor control of their blood sugar levels or blood pressure and those who have had diabetes for many years – these people should also be screening more regularly.
Treatment

Patients with proliferative diabetic retinopathy require more aggressive treatment to stop the growth of new, fragile blood vessels in the retina. This can be achieved using a procedure known as laser photocoagulation. This procedure uses short bursts of laser light fired into the eye at these new, developing vessels to stop them from growing. Laser photocoagulation has been very effective in stopping diabetic retinopathy from progressing to blindness.
In the last few years, the use of a new treatment called anti-vascular endothelial growth factor (anti-VEGF) therapy has also been very successful in treating proliferative diabetic retinopathy. Anti-VEGF drugs are injected into the affected eye and can act directly on these blood vessels to stop them from growing. Often a combination of laser therapy and anti-VEGF therapy is used for diabetic retinopathy or for macular oedema.
In extreme cases, diabetic retinopathy that doesn’t improve with laser photocoagulation therapy may require a surgical procedure on the eye to remove the blood due to these bleeding retinal vessels, called a vitrectomy. This procedure can also allow a detached retina to be repaired.
References
- American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2012; 35 Suppl 1:S64-71. [Abstract | Full Text]
- Diabetes prevalence in Australia: detailed estimates for 2007-08 [online]. Canberra, ACT: Australian Institute of Health and Welfare; 2011 [cited 17 July 2012]. Available from: URL link
- Devendra D, Liu E, Eisenbarth G. Type 1 diabetes: recent developments. BMJ. 2004; 328: 750-754. [Abstract | Full Text]
- Bryant W, Greenfield J, Chisholm D, Campbell L. Diabetes guidelines: easier to preach than to practise? A retrospective audit of outpatient management of type 1 and type 2 diabetes mellitus. MJA. 2006; 185 (6): 305-309. [Abstract | full Text]
- Kumar P, Clark M (eds). Clinical Medicine (5th edition). Edinburgh: WB Saunders Company; 2002. [Book]
- Sloan FA, Bethel MA, Ruiz D Jr, et al. The growing burden of diabetes mellitus in the US elderly population. Arch Intern Med. 2008; 168(2): 192-9. [Abstract | Full Text]
- Braunwald E, Fauci AS, Kasper DL, et al. Harrison’s Principles of Internal Medicine (15th edition). New York: McGraw-Hill Publishing; 2001. [Book]
- Yau JW, Rogers SL, Kawasaki R, et al. Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care. 2012; 35(3): 556-64. [Abstract | Full Text]
- Ockrim Z, Yorston D. Managing diabetic retinopathy. BMJ. 2010; 341: c5400. [Abstract]
- Mitchell P, Foran S. Guidelines for the management of diabetic retinopathy [online]. Canberra, ACT: National Health and Medical Research Council; 2008 [cited 28 February 2011]. Available from: URL link
- Tremolada G, Del Turco C, Lattanzio R, et al. The role of angiogenesis in the development of proliferative diabetic retinopathy: impact of intravitreal anti-VEGF treatment. Exp Diabetes Res. 2012; 2012: 728325. [Abstract | Full Text]
- Fenwick EK, Pesudovs K, Rees G, Dirani M, Kawasaki R, Wong TY et al.
- The impact of diabetic retinopathy: understanding the patient’s perspective. Br J Ophthalmol. 2011; 95(6):774-82. [Abstract]
- Hirai FE, Tielsch JM, Klein BE, Klein R. Ten-year change in vision-related quality of life in type 1 diabetes: Wisconsin epidemiologic study of diabetic retinopathy. Ophthalmology. 2011; 118(2): 353-8. [Abstract | Full Text]
- American Diabetes Association. Standards of medical care in diabetes–2012. Diabetes Care. 2012; 35 Suppl 1: S11-63. [Abstract | Full Text]
- Facts about diabetic retinopathy [online]. Bethesda, MD: National Eye Institute; October 2009 [cited 22 February 2011]. Available from: URL link
- Gong Q, Gregg EW, Wang J, et al. Long-term effects of a randomised trial of a 6-year lifestyle intervention in impaired glucose tolerance on diabetes-related microvascular complications: the China Da Qing Diabetes Prevention Outcome Study. Diabetologia. 2011; 54(2): 300-7. [Abstract | Full text]
- Gaede P, Lund-Andersen H, Parving HH, Pedersen O. Effect of a multifactorial intervention on mortality in type 2 diabetes. N Engl J Med. 2008 Feb 7; 358(6): 580-91. [Abstract | Full Text]
- Spurling G, Askew D, Jackson C. Retinopathy: Screening recommendations. Aust Fam Physician. 2009; 38(10): 780-3. [Abstract | Full text]
- Stewart MW. Chapter 1: Pathophysiology of diabetic retinopathy. In: Browning DJ (ed). Diabetic Retinopathy: Evidence-based management. New York: Springer; 2010: 1-31. [Book]
- Wirostko B, Beusterien K, Grinspan J, et al. Patient preferences in the treatment of diabetic retinopathy. Patient Prefer Adherence. 2011; 5: 229–237. [Abstract | Full Text]
- Lamoureux EL, Tai ES, Thumboo J, Kawasaki R, Saw SM, Mitchell P, Wong TY. Impact of diabetic retinopathy on vision-specific function. Ophthalmology. 2010; 117(4):757-65. [Abstract | Full Text]
- Coyne KS, Margolis MK, Kennedy-Martin T, et al. The impact of diabetic retinopathy: perspectives from patient focus-groups. Fam Prac. 2004; 21(4): 447-53. [Abstract]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.