- What is Coronary Heart Disease (CHD)
- Statistics on Coronary Heart Disease (CHD)
- Risk Factors for Coronary Heart Disease (CHD)
- Progression of Coronary Heart Disease (CHD)
- Symptoms of Coronary Heart Disease (CHD)
- Clinical Examination of Coronary Heart Disease (CHD)
- How is Coronary Heart Disease (CHD) Diagnosed?
- Prognosis of Coronary Heart Disease (CHD)
- How is Coronary Heart Disease (CHD) Treated?
- Coronary Heart Disease (CHD) References
What is Coronary Heart Disease (CHD)
- angina (stable and unstable)
- myocardial infarction (heart attack)
- heart failure
- arrhythmias (irregular heart beats)
- and sudden death
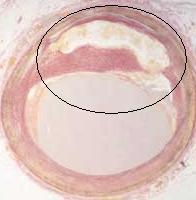
The image above is that of a cross section of an artery effected by fatty deposits along its length.
Statistics on Coronary Heart Disease (CHD)
Coronary heart disease is more common than what we think. In Australia it is now considered one of the biggest killers. Together with stroke and vascular diseases in a group, coronary heart disease kills more Australians than any other disease group. Around 3.6 million Australians are affected by heart, stroke and vascular diseases and the number continues to increase with a greater proportion of the population becoming overweight.
Aboriginal and Torres Strait Islander peoples, compared to other Australians, are 2.6 times as likely to die from heart, stroke and vascular diseases. They are more likely to smoke, have high blood pressure, be obese, have diabetes, drink excessive alcohol, and have end-stage renal disease. These are all risk factors for the disorder and poor outcomes.
Worldwide similar figures are emerging with 13.7 million people in the United States having CHD. In the United Kingdom 1.3 million people have angina and an estimated 330 000 people have a heart attack each year.
Risk Factors for Coronary Heart Disease (CHD)
Factors that predispose someone to coronary heart disease can be divided into modifiable ones and non-modifiable ones.Modifiable risk factors:
- Smoking
- Hypertension
- Diabetes Mellitus
- High cholesterol
- Obesity and sedentary lifestyle
- Heavy alcohol consumption
- Oral contraceptive pill
Non-modifiable risk factors:
- Age
- Male gender (women before the menopause have protection of the heart from oestrogen hormones)
- Family history of coronary heart disease
Statistics
- 90% of Australian adults have at least one modifiable risk factor, while 25% have three or more risk factors
- 60% of Australian adults are overweight
- 54% are not sufficiently active to achieve health benefits
- 51% have high blood cholesterol
- 30% have high blood pressure
- 20% smoke daily
- 10% drink at levels considered harmful to their health
- 8% have diabetes
The numbers of people who are overweight, not active enough, and have diabetes have increased significantly over the last 10-20 years. However, the rate of smoking and high blood pressure has fallen in the last 10-20 years.
Progression of Coronary Heart Disease (CHD)
The presence of clinical atherosclerosis in vessels supplying the heart generally indicates an increased likelihood that it exists elsewhere since the risk factors are generally the same.
A study showed that among participants who had an initial heart attack, 21 percent of men and 25 percent of women had preceding angina pectoris. Approximately 10 percent had prior intermittent claudication, 5 to 8 percent a stroke, and 3 to 10 percent heart failure.
All the major risk factors (eg, hypertension, high cholesterol, diabetes mellitus, smoking) impact significantly on the rate of development of coronary and peripheral artery disease. After an MI, possible complications that may develop include arrhythmias (irregular heart beat), ischaemia (insufficient blood flow to the heart) and impaired heart chamber function.
Symptoms of Coronary Heart Disease (CHD)
The diagnosis of coronary heart disease can often be made following a thorough history by a doctor. The doctor wil be particluarly interested in any chest pain, its site, any spreading into the jaw, neck or arms and whether the pain is made worse by exercise. Usually cardiac pain will be experienced as a crushing central chest pain, worse on exertion and relieved by rest. Anginal pain usually lasts less than 20 minutes and pain associated with a heart attack lasts 15-20 minutes.
Associated symptoms include, shortness of breath, nausea and vomiting. Occasionally a heart attack may be painless (called a silent heart attack) especially if you have diabetes.
Other important questions will be asked by the doctor such as whether anyone else in your family suffers from heart disease or if you have other medical conditions that can predispose to coronary heart disease. You should remember that chest pain may indicate a serious disorder so if you experience this problem, you should seek medical advice urgently.
Clinical Examination of Coronary Heart Disease (CHD)
A full physical examination needs to be performed when someone is suspected of having coronary heart disease. The doctor will check the temperature (to exclude infective cause of chest pain), respiratory rate (some patients may be breathless), pulse rate (for rate and regularity) and blood pressure (as high blood pressure is a risk factor for coronary heart disease).
A cardiovascular examination will be performed to assess the heart function (e.g. for the presence of heart failure, valvular disease) and the presence of peripheral vascular disease.
The respiratory system will also be assessed to rule out lung diseases causing similar complaints (chest pain, breathlessness).
How is Coronary Heart Disease (CHD) Diagnosed?
Investigations for coronary heart disease include a series of blood tests including a full blood count to determine whether anaemia is present, cardiac enzymes (measures substances released following damage to the heart muscle), lipid profile and thyroid tests if indicated (as hyperthyroidism can cause angina). An heart tracing (electrocardiography, ECG) and a chest X-ray will also be performed.
Prognosis of Coronary Heart Disease (CHD)
In general, the prognosis of coronary heart disease is related to the number of affected vessels (one-, two- or three vessel coronary artery disease) and the degree of dysfunction of the left ventricle (the heart chamber that pumps out blood to the rest of the body other than the lungs). A patient with a single affeted vessel and good left ventricular function has an excellent outlook (5-year survival >90%), whereas a patient with severe left ventricular dysfunction and extensive disease involving three vessels has a poor porgnosis (5-year survival
At six years following a recognized MI, men have a two-fold increase in the age-adjusted risk of a recurrence, a four-fold increase in the risk of developing angina, a five-fold increase in the risk of heart failure, and more than a two-fold increase in the risk of stroke. For women, the age-adjusted outlook is substantially worse for all of the events except angina. Adjusted to an average age of 50, the survival at 15 years without any further heart problems in those with a diagnosed heart attack is about 44 percent. The death rate for all patients who are hospitalised for definite or probable heart attack is about 10% in women and 9% in men.
How is Coronary Heart Disease (CHD) Treated?
If you experience an anginal attack you will be treated immediately with morphine (for chest pain), oxygen, nitrates (to open up the vessels around the heart) and aspirin or clopidogrel to reduce the risk of heart attack.
More invasive options are percutaneous coronary intervention (PCI) and coronary artery bypass grafting (CABG) are sometimes required. PCI aims to open up a coronary artery (blood vessel that brings blood and oxygen to the heart muscle) and restore blood flow, usually with a balloon inserted by a catheter through the femoral artery in the groin area. CABG is an “open heart” surgery where the saphenous vein from the leg is used to carry blood around the obstruction in the heart.
A heart attack is a medical emergency and requires urgent treatment to allow survival. If you experience prolonged chest pain do not hesitate to seek medical care. For acute heart attack, early management comprises:
- High flow oxygen.
- Pain relief (usually morphine) and medication to stop vomiting.
- Aspirin plus thrombolysis (to break off the clot) or primary PCI.
- Detection and management of acute complications: arrhythmia (irregular heart beat), ischaemia, heart failure. It is likely you will be monitored carefully with an ECG to detect complications. If an arrhythmia occurs defibrillation may be required.
In summary, patients with established CHD (and all patients as a primary preventative measure) are encouraged to:
- Stop smoking.
- Exercise more.
- Lose weight if overweight.
- Reduce or control blood pressure.
- Control diabetes.
- Control lipid (fat) levels and cholesterol.
Management will depend on your underlying risk factors and treatments may vary across individuals. Long-term aspirin (an anti-platelet medication) has shown to be beneficial in reducing recurrent heart attack and mortality in several clinical trials and is recommended in virtually all patients. All individuals who have experienced a heart attack or are known to suffer coronary heart disease should be prescribed short-acting nitrate sprays. An action plan for the event of future chest pain will be explained to you by your doctor.
If chest pain occurs patients should:
- Rest and administer the short-acting nitrates.
- Take some aspirin (between 150 and 300mg) unless you have contraindications for this medication.
- Call an ambulance (dial 000) if chest pain/discomfort not completely relieved in 10 to 15 minutes. If ambulance services are not available where you live you will be given a designated clinician who you should call.
With early and effective management the risk of death from acute heart attack and future sequelae are markedly reduced.
Coronary Heart Disease (CHD) References
- Acute Coronary Syndrome Guidelines Working Group, Guidelines for the management of acute coronary syndromes. MJA 2006; 184 (8): S1-S32.
- American Heart Association. Heart and Stroke Facts: 1995 Statistical Supplement. American Heart Association 1994.
- Australian Institute of Health and Welfare (AIHW) 2004. Heart, stroke and vascular diseases – Australian facts 2004. AIHW Cat. No. CVD 27. Canberra: AIHW and National Heart Foundation of Australia (Cardiovascular Disease Series No. 22).
- Cotran RS, Kumar V, Collins T. Robbins Pathological Basis of Disease Sixth Ed. WB Saunders Company 1999.
- Cupples, LA, Gagnon, DR, Wong, ND, et al. Pre-existing cardiovascular conditions and long-term prognosis after initial myocardial infarction: the Framingham Study. Am Heart J 1993; 125:863.
- Haslett C et al. editors. Davidson’s Principles and Practice of Medicine. 19th ed. Edinburgh ; New York : Churchill Livingstone; 2002.
- Lampe, FC, Whincup, PH, Wannamethee, SG, et al. The natural history of prevalent ischaemic heart disease in middle-aged men. Eur Heart J 2000; 21:1052.
- Murtagh J. General Practice, 3rd Ed. McGraw-Hill, Australia, 2003.
- National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand. Reducing Risk in Heart Disease 2004. Guidelines for Preventing Cardiovascular Events in People with Coronary Heart Disease. Heart Fundation, 2004. Available at URL: http://www.heartfoundation.com.au/downloads/RRIHD_fullguide_update_010405.pdf
- Rosamond, WD, Chambless, LE, Folsom, AR, et al. Trends in the incidence of myocardial infarction and in mortality due to coronary heart disease, 1987 to 1994. N Engl J Med 1998; 339:861.
- Smith et al. ‘Principles for National and Regional Guidelines on Cardiovascular Disease Prevention- A Scientific Statement from the World Heart and Stroke Forum,’ American Heart Association 2004. DOI: 10.1161/01.CIR.0000133427.35111.67.
- Vaccarino, V, Krumholz, HM, Berkman, LF, Horwitz, RI. Sex differences in mortality after myocardial infarction. Circulation 1995; 91:1861.
- Wilson PWF. Epidemiology and prognosis of coronary heart disease. UpToDate 2005. Available at URL: http://www.utdol.com/application/topic.asp file=chd/64193&type=A&selectedTitle=2~429
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







