Jump To
- Introduction
- Common types of headaches
- How physiotherapy can help
- When to see a doctor: ‘Red flags’
- References
Introduction
Headaches are one of the most common health conditions in Australia. It is likely that all of us will experience headaches at some stage, and at any given time, 15% of us are taking pain relief medications for a headache.1
Headaches can be categorised into two broad groups: primary and secondary.1 Primary headaches are caused by problems with pain-sensitive structures in the head, and are not due to an underlying illness elsewhere in the body.2 Secondary headaches, on the other hand, are a symptom of an underlying condition, such as an infection, injury or tumour.1
| · Headaches are one of the most common health conditions in Australia.
· There are many types of headaches. Two of the most common are tension headaches (triggered by emotional and physical stress) and neck headaches (caused by an underlying neck issue). · Often, headaches are caused by multiple factors. These often include lifestyle factors such as stress, sleeping positions, posture, work habits and exercise habits. · Physiotherapy treatment techniques such as manipulation, massage, postural correction and rehabilitation exercises can help manage some common types of headaches. Physiotherapists can also provide useful advice on how to prevent headaches by modifying everyday habits. · You should visit your doctor if you are experiencing any of the ‘red flags’, or if you have any concerns in general. |
Common types of headaches
Tension headaches are the most common type of headache, affecting two out of three Australians at some stage during their lifetime. Tension headaches are often described as involving the feeling of a tight band around the head and are often associated with muscle tightness in the head, neck or jaw.1
Tension headaches can be due to physical and/or emotional stress. Poor posture, and muscle tension in the back, shoulders and neck can cause referred pain in the head. Emotional stress is believed to trigger our ‘fight or flight’ response, resulting in the release of ‘stress chemicals’ such as adrenaline. This can further tighten the muscles of the back, shoulders, neck and head, lower a person’s pain tolerance and reduce the amount of the body’s natural pain-relieving chemicals (eg. endorphins).1
Find and instantly book affordable physios within AustraliaGet on top of your physical health
Neck headaches – often referred to as cervicogenic headaches – result from pain referred from an underlying neck issue.
There are many pain-sensitive structures that exist at the junction of the upper neck (cervical) and back of head (occipital) regions. These structures – including the lining of the cervical spine, the joints, ligaments, cervical nerve roots and surrounding muscles – can cause pain in the presence of an underlying issue.3 The features of neck headaches can be similar to those of tension headaches or migraines, often making it difficult to distinguish between them.4
Cluster headaches are considered to be one of the most painful types of headaches. They often awaken people in the middle of the night with intense pain in, behind, or around the eye on one side of the head.5
The cause of cluster headaches is not clear; however, due to the typical patterns seen, it is suggested that the hypothalamus (the body’s biological clock) might play an important role. Unlike tension headaches and migraines, there doesn’t appear to be a link between cluster headaches and triggers such as stress, foods or hormonal changes.5
Migraines can result in severe throbbing or pulsing pain, usually on one side of the head. This is often associated with other symptoms, such as nausea, vomiting and sensitivity to both light and sound. Migraines can also occur with aura, which are disturbances of the nervous system. Examples of aura include experiencing flashes of light or blurred vision (visual disturbances), hearing noises or music (auditory disturbances), having pins and needles in a limb (sensory disturbances) and difficulty speaking (verbal disturbances). 6
The causes of migraines are not well understood; however, it appears that genetics and environmental factors play an important role. Suggested causes include alterations in the brainstem and its interactions with the trigeminal nerve (an important pain pathway); and imbalances in brain chemicals, particularly serotonin.6 A number of factors can trigger migraines in different people. These include: certain foods (eg. salty or processed foods), stress, changes in sleeping patterns, exposure to sensory stimuli (eg. bright lights and sun glare) and certain medications (such as glyceryl trinitrate, which is commonly used to treat angina).6
How physiotherapy can help
Physiotherapists are experts in posture and movement of the body and are well-placed to diagnose, manage and prevent some of the common types of headaches.7
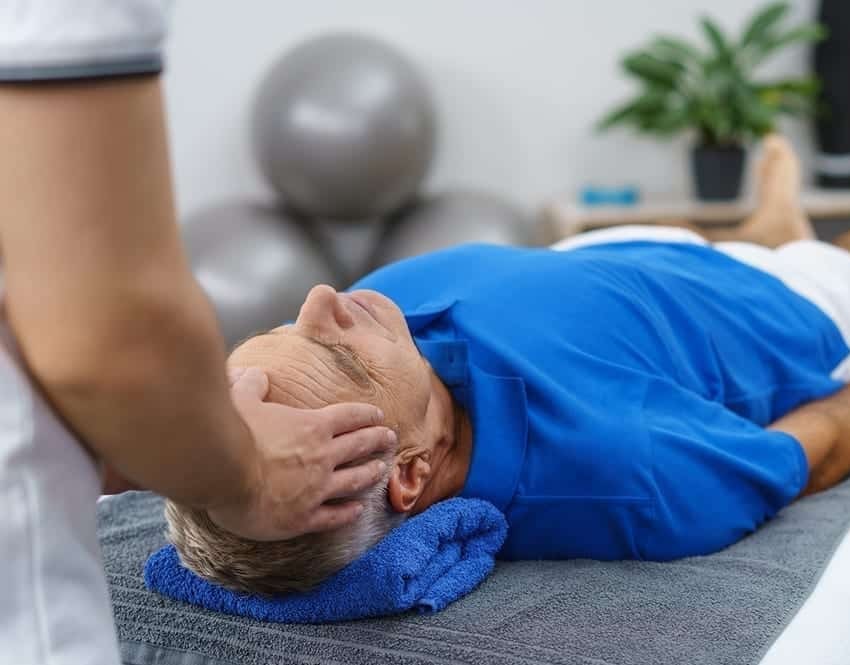
Physiotherapists will be able to determine, for example, if issues with the soft-tissue in your neck are contributing to your headaches. In this case, you could benefit from specific physiotherapy for neck headaches, which might include techniques such as manipulation, functional and rehabilitation exercises, postural assessment and correction, relaxation therapy, massage and mobilisation.7
Your physiotherapist can also provide advice on ways to help prevent and manage some of the common underlying causes of headaches by focusing on different aspects of your lifestyle. Examples include:7
- Posture – Your posture is very important. Think tall with your chest lifted, shoulders relaxed, head level and chin tucked in.
- Work – Avoid working with your head down for long periods of time, and frequently stretch and change positions.
- Sleeping – Poor sleeping positions can strain your neck. Your physiotherapist can advise you on which type of pillow may be best for you.
- Exercise – Your physiotherapist can show you specific exercises that help with tight or weak muscles and can help you to restore normal function.
- Relaxation – Learning to recognise when you are tense is an important component of tension headache physiotherapy. Your physiotherapist can show you a range of relaxation techniques that can help manage this.
Your physiotherapist will often work closely with your local GP, particularly in the case of complex headaches. Physiotherapy for migraines, for example, won’t often be recommended until after you have seen your doctor.7
When to see a doctor: ‘Red flags’
There are some features of headaches – called ‘red flags’ – that require urgent attention.8 Your doctor might need to order special tests to find out if there is an underlying cause requiring medical care. These features include (but are not limited to):8
- New onset headaches that occur during pregnancy
- New onset headaches for those with a medical history of cancer, HIV infection or head trauma
- Headaches that come on suddenly
- Headaches that become progressively worse, or persist despite pain relief
- Headaches associated with vision changes, weakness in your limbs, or any other nervous system signs (for migraine sufferers, this includes any signs or symptoms that aren’t typical for you)
- Any headache that feels unusual for you
If you have any concerns about your headache, it is strongly recommended that you visit your local health professional.
A: Use HealthEngine to find and book your next Physiotherapist appointment. Click on the following locations to find a Physiotherapy clinic in your state or territory.
This article is for informational purposes only and should not be taken as medical advice. If in doubt, HealthEngine recommends consulting with a registered health practitioner.
References
- Better Health Channel (online). Headache [accessed 19 Mar 2019]. Available from: URL link
- Mayo Clinic (online). Headache [accessed 19 Mar 2019]. Available from: URL link
- American Migraine Foundation (online). Cervicogenic headache [accessed 19 Mr 2019]. Available from: URL link
- Biondi, D.M., 2005. Cervicogenic headache: a review of diagnostic and treatment strategies. The Journal of the American Osteopathic Association, 105(4_suppl), pp.16S-22S. Available from: URL link
- Mayo Clinic (online). Cluster headache [accessed 19 Mar 2019]. Available from: URL link
- Mayo Clinic (online). Migraine [accessed 19 Mar 2019]. Available from: URL link
- Australian Physiotherapy Association (online). Headache: physiotherapy [accessed 19 Mar 2019]. Available from: URL link
- Joubert, J., 2005. Diagnosing headache. Australian family physician, 34(8), p.621. Available from: URL link
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.