- What are burns?
- Statistics on burns
- Risk factors for burns
- Progression of burns
- Symptoms of burns
- Clinical examination of burns
- How are burns diagnosed?
- Prognosis of burns
- Treatment of burns
- References
What are burns?
Burns are injuries to body tissues that can result from heat, electricity, radiation, or chemicals. Burns are most commonly caused by heat (thermal burns), including fire, steam, tar, or hot liquids. Burns can also be caused by chemicals, which are similar to thermal burns, whereas burns caused by radiation and electricity can cause different injuries and outcomes.
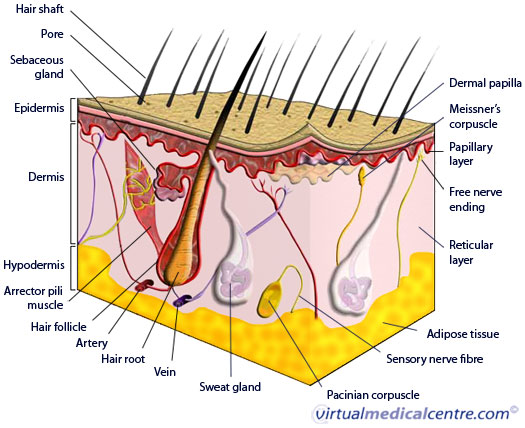
Thermal and chemical burns often occur when heat or chemicals come in direct contact with part of the body, most commonly affecting the skin. In most situations, the skin sustains most of the damage. However in deeper burns, the underlying structures such as fat, muscle and bone may also be affected.
When the body’s tissues sustain a burn injury, fluid leaks into the tissues from the blood vessels, resulting in swelling and pain. Depending on the depth of the burn, the skin may turn red, ulcerate, blister or be completely destroyed. A complication of damaged skin involves infection – the skin’s natural function as the body’s barrier is breached and invading organisms can enter the body.
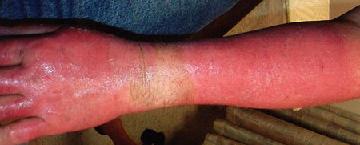
Statistics on burns
Approximately 1% of the Australian and New Zealand population will suffer from a burn each year. Of these people affected, 50% will suffer from some daily restriction of activity and 10% will require admission to hospital.
Exposure to heat is the most common cause of a burn accounting for over half of all burn cases. Chemical exposure accounts for 2.1-6.5% of all admissions to burn units. Electrical burns are estimated to account for 3-4% of burn related injuries.
Risk factors for burns
Those people who are predisposed to burns include:
- If you work with chemicals, electricity or hot substances (fire, heat, steam);
- The elderly and children are more likely to sustain burns. They may have a delayed reaction to exposure to hot substances or chemicals. The elderly may suffer from memory problems with advancing age and be more at risk for burns;
- If you have an increased level of alcohol consumption;
- If you have a psychiatric disorder, you may be at increased risk;
- If you have a neurological disease such as stroke or are unable to move your limbs, you may be more at risk for burns.
Patients at higher risk for hospital admission include those with:
- Burns affecting more than 10% of total body surface area;
- Burns of special areas such as the face, hands, feet, genitals;
- Full thickness burns;
- Electrical and chemical burns;
- Burns where there is an associated inhalational injury;
- Burns involving the whole circumference of the limbs or other parts of the body;
- Burns in patients with pre-existing medical conditions;
- Burns in patients with associated trauma.
Progression of burns
Most minor burns are superficial and do not cause complications. However, deep partial thickness and full thickness burns are associated with increased swelling and take more time to heal. Additionally, deeper burns can cause scar tissue to form. This scar tissue shrinks and can contract the overlying skin, as it heals.
Severe burns can cause complications related to excessive loss of body fluids and tissue damage. Complications from severe burns may develop many hours later. The longer the complication is present, it is more likely to cause more severe complications. Younger children and older adults tend to be more seriously affected by complications.
Symptoms of burns
If you are affected by burns, the doctor may ask you some of the following questions to try and determine the cause, complications and appropriate treatment to arrange.
- Where were you when you sustained the burn and how did it occur?
- Are there any other injuries you sustained?
- What time did the accident occur?
- What type of substance did you come in contact with?
- Did the accident occur in a closed space?
- Were you wearing any clothing?
- Have you got any pre-existing medical conditions or are you on any regular medications?
- Were there any other witnesses to the burn?
- Have you applied any treatment to the burn?
- How does the burn feel (painful, non-painful)?
- Are there other symptoms such as wheezing, change in your voice, difficulty breathing, dark mucus?
Clinical examination of burns
When the doctor examines you, he or she may try to identify the following information about your burn.
- Location of injury;
- Body surface area (BSA) affected;
- Depth of burn.
Location of injury
Burns affecting special areas such as the face, hands, feet, genitalia and major joints are more likely to result in long term complications, thus if you have sustained burns identified in these areas, you may be more likely to require hospital admission.
Body surface area (BSA) affected
It is important to have an idea of how much of your body is affected by the burns process, to allow the doctor to determine the type of management that is needed. The percentage of your body surface area affected is commonly calculated using one of the following methods:
- Wallace’s Rule of Nines: With this rule, your head and neck accounts for 9% of your BSA, each arm 9%, anterior part of the chest – 2 x 9% (18%), posterior trunk 2 x 9%(18%), each leg 2 x 9% (18%), and 1% for your perineum (the area around the anal area);
- Area of your hand: this is approximately 1% of BSA;
- Lund and Browder charts: these are special burn charts usually available in the emergency departments. These charts are filled in and the percentage burn estimated using the instructions on the charts.
Depth of burn
The depth of burn injuries is particularly important especially if the burn is causing decreased oxygen supply to the end digits of the body or difficulties with chest expansion and breathing. Burns can be divided into:
- Superficial burns;
- Partial thickness burns (mid-dermal);
- Partial thickness burns (deep-dermal);
- Full-thickness burns.
Superficial burns
These burns are usually red, moist and very painful. The outermost layer of the skin is involved (the epidermis) and there may be blisters present. Healing generally occurs within 7-10 days with minimal or no scarring.
Partial-thickness burns
- Mid-dermal: The outermost layer of skin in lost, as well as parts of the dermis (the next layer of skin). The burn is pink in colour, with small white patches. The skin still blanches on pressure and is painful. Healing occurs in 7-14 days depending on the degree of skin destruction. Some mild pigmentation or scarring may result.
- Deep-dermal burns: Here there is deeper dermal destruction. The burn appears white and does not blanche on pressure. The skin is insensitive and takes a longer period of time to heal, with scarring.
Full-thickness burns
Full thickness burns extend deep down into the dermis. The burn is leathery, ranges in colour from white/gray/black and is non-painful. There is loss of sensation and it does not blanch on pressure. Healing occurs from around the edges of the surrounding skin but the process is slow, with scarring and contracture.
How are burns diagnosed?
When you have suffered a severe burn, the doctor may order some of the following tests. Blood is taken from your arm, for:
- Full blood picture;
- Urea & electrolytes;
- Arterial blood gases with carboxyhaemoglobin;
- Coagulation profile;
- Blood for cross match and group and hold.
The urine is also analysed for creatinine phosphokinase and urine myoglobin, which are substances that may be released by the muscles and heart, especially in electrical injuries.
Some imaging studies that may be considered include:
- A chest x-ray may be performed if there is the possibility that you have sustained an inhalation injury;
- Other x-rays may be ordered if you have any other associated injuries;
- CT scans may be performed to identify other accompanying injuries.
Prognosis of burns
Superficial burns heal in days to weeks without scarring. Deeper partial thickness burns take weeks to heal and may be associated with scarring. Full thickness burns require skin grafting. Burns that involve more than 90% of the body surface, or more than 60% in an elderly person, are usually fatal.
Treatment of burns
First aid for minor burns
- It is important to calm and reassure the burnt patient;
- If the skin is unbroken, cool water should be run over the affected area or the area should be soaked in a cool water bath (not ice cold) for at least 20 minutes;
- The burn should then be covered with a dry, sterile bandage, clean dressing or plastic covering such as cling wrap;
- Simple analgesics such as non-steroidal anti-inflammatories (ibuprofen) or paracetemol can help relieve pain and swelling’
- It is recommended that you should visit a health professional as soon as possible – superficial burns usually heal without further treatment. However, deeper or larger burns, or those located on special areas (hands, feet, face, groin) may require further treatment;
- Your tetanus immunisation status should be checked and up to date.
First aid for major burns
- If someone is on fire, they should follow the instructions to STOP, DROP, and ROLL. The burnt patient should be wrapped in a thick material / blanket to smother the flames and extinguished with water;
- The emergency number 000 should be dialed and an ambulance called;
- Before the burns are treated, the burning agent must be stopped from inflicting further damage. Burnt or smothering clothing or those soaked with chemicals should be immediately removed;
- Next, resuscitation according to the ABC’s – Airway, Breathing and Circulation should be promptly commenced. Ensure that the burnt patient’s airway is not blocked. If there is any obstruction, attempts to open the airway by laying them on the side, using a head tilt and chin lift should be commenced;
- Next, the person’s breathing should be checked. If there is absence of breath sounds and no chest wall movement, rescue breathing and/or CPR should be commenced;
- The burnt area should be covered with a clean cloth and any blisters should remain intact. The burnt body part should be protected from pressure and friction;
- You should continue to monitor the patient’s vital signs including their pulse, breathing rate and blood pressure, until medical help arises.
Hospitalisation is sometimes necessary for optimal care of burn injuries. In the hospital setting, treatment such as elevating a severely burned limb above the level of the heart to prevent swelling, is more easily accommodated. In addition, burns that affect special areas may be best managed under expert advice, to ensure that essential daily functions, such as walking or eating, are preserved.
With superficial burns, topical treatments such as silver sulfadiazine cream are applied to the affected areas. This cream helps prevent infection and forms a seal to prevent further bacteria from entering the wound. A sterile bandage or gauze may be applied to protect the burned area from soil and further injury.
With more severe burns, the patient may be dehydrated and require large amounts of fluid, which are best given through the veins. Destruction of muscle tissue is also managed with administering large amounts of fluid. This helps dilute the myoglobin in the blood, preventing damage to the kidneys. Ensuring that the burnt area is kept clean is also important, to prevent development of infection. This is best achieved by gently cleaning the burns with sterile water and changing the bandages on a regular basis.
References
- Devitt P, Barker J, Mitchell J. Clinical Problems in General Medicine & Surgery. Australia: Harcourt Brace Jovanovich Group Pty Ltd, 2003 [Book]
- Hettiaratchy S, Papini R. Initial management of a major burn: II-assessment and resuscitation. BMJ, 2004; 329: 101 – 103 [Full text]
- Jones S, Gilbert P. Immediate Care of the Burned Patient. Journal of Surgery (Oxford). 2005 [Abstract]
- Goodis J, Adler J. Thermal Burns in Emergency Medicine. Medscape Reference [serial online]. 2010 [cited 3 June 2011]. Available from: [URL link]
- RPH Burns Management Team, Burns Management Resource Material.Australia: Smith & Nephew; 2005
- Cox, R. Chemical Burns in Emergency Medicine. Medscape Reference [serial online]. 2010 [cited 3 June 2011]. Available from [URL link]
- Hettiaratchy S, Dziewulski P. ABC of Burns: Introduction. BMJ. 2004;328(7452):1366-8 [Full text]
- Kreisfeld R, Harrison JE. Injury Research and Statistics Series Number 55: Hospital separations due to injury and poisoning 2005-06. AIHW. 2010, Cat. no. INJCAT 131. Available from: [URL link]
- HenleyG, Harrison JE. Injury research and statistics series no 51: Injury deaths, Australia 2004–05. AIHW. 2009, Cat. no. INJCAT 127. Available from: [URL link]
- Hettiaratchy S, Dziewulski P. ABC of Burns: Pathophysiology and types of burns. BMJ. 2004;328(7453):1427-9. [Full text]
- Benson A, Dickson WA, Boyce DE. ABC of Wound Healing: Burns. BMJ. 2006;332(7542):649-52. [Full text]
- Papini R. Management of Burn injuries of various depths, BMJ. 2004;329(7458)158-60. [Abstract]
- Colquhoun M, Handley A, Evans TR. ABC of Resuscitation (5th edition). United Kingdom: BMJ Books; 2004.
- Wasiak J, Spinks A, Asby K et al. The epidemiology of burn injuries in an Australian setting, 2000–2006. Burns. 2009;35(8):1124-32. [Abstract]
- Gangemi EN, Gregori D, Berchialla P et al. Epidemiology and risk factors for pathologic scarring after burn wounds. Arch Facial Plast Surg. 2008; 10(2):93-102. [Full text]
- Ladak A, Tredget EE. Pathophysiology and Management of the Burn Scar. Clin Plast Surg. 2009;36(4):661-74. [Abstract]
- Bloemen MC, van der Veer WM, Ulrich MM et al. Prevention and curative management of hypertrophic scar formation. Burns. 2009; 35(4)463-75. [Abstract]
- Mustoe TA, Cooter RD, Gold MH et al. International clinical recommendations on scar management. Plast Reconstr Surg. 2002:110(2):560-71. [Abstract]
- Blot S, Brusselaers N, Monstrey S et al. Development and validation of a model for prediction of mortality in patients with acute burn injury. Br J Surg. 2009:96(1):111-7.
- Spanholtz TA, Theodorou P, Amini P et al. Severe Burn Injuries: acute and long-term treatment. Dtsch Arztebl Int. 2009;106(38):607-13.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.