- Introduction to breast pain
- Statistics on breast pain
- Causes of breast pain
- Impact of breast pain
- At the doctor’s office
- Investigations
- Treatment
Introduction to breast pain
Mastalgia or breast pain is commonly encountered by women. It is thought to be present in up to 69% of women and is most common in women between the ages of 30 and 50.
Breast pain may be due to normal cyclical changes in hormone levels or due to certain diseases. Cyclical hormonal changes are the most common cause of breast pain but a doctor should always be consulted to determine the cause of this symptom. Breast cancer is rarely the cause of breast pain, only accounting for 1.2–6.7% of cases of this symptom.
Statistics on breast pain
Studies have shown that almost 50% of women have consulted a health care professional due to mastalgia. It is also the most common breast-related symptom which prompted a visit to a health care professional. Amongst which, women who are under the age of 35 are most likely to have a mammogram (x-ray of both breasts) as part of ongoing investigations.
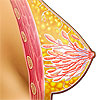 |
For more information, see Anatomy of the Breast. |
Causes of breast pain
Cyclical hormonal changes due to menstrual cycle
Breast pain associated with the hormonal changes of the menstrual cycle is usually cyclical in nature and varies with the time of the month. One third of women may, however, have noncyclical pain (not related to the menstrual cycle) which is less responsive to treatment.
Physiological breast pain typically presents in the premenstrual period (usually 1 week prior to onset of menses). It most frequently affects both breasts and is usually worse in the upper outer quadrant of the breasts. This type of breast pain is also typically associated with fibrocystic changes. Fibrocystic changes of the breast are non-cancerous tumours caused by hormonal changes during the menstrual cycle and usually resolve after menopause (the cessation of periods for 2 years or more occurring at an average age of 51).
Hormonal therapies/drug side effects
Breast pain is one of the most frequently encountered side effects of hormonal therapies such as the oral contraceptive pill in women of reproductive age and hormonal replacement therapy in menopausal women. Other commonly encountered side effects of hormonal therapy include unwanted bleeding, headaches, pimple break-outs, decrease in sex drive and weight changes.
Theophylline (sold, for example, as Aminophylline and Nuelin), a drug sometimes used for the treatment of long-term asthma, may also rarely cause breast discomfort/pain. In addition, spironolactone (for example, sold under the trade names Aldactone and Spiractin), which is a drug used in people suffering from heart failure, can also cause gynaecomastia (breast enlargement) in males and breast pain in females.
Breast diseases
Mammary duct ectasia
Mammary duct ectasia is a condition caused by enlargement of the milk ducts present in breasts. It may cause you to experience fever, breast pain/ tenderness and nipple discharge.
It is most common amongst women between 40 and 50 years of age and may sometimes not cause any symptoms. Mammary duct ectasia usually requires no treatment and is not a risk factor for breast cancer.
Mastitis
Mastitis refers to inflammation of the breast which is caused mainly by milk stasis (stagnant milk) or infections. Milk being stagnant is usually the initial cause of mastitis which can then progress to an infection. Infections of the breast such as mastitis and formation of abscesses (collections of pus) within breast tissue are common among mothers who are breastfeeding. It is most common in the first month of breastfeeding and is usually caused by obstruction of the milk ducts leading to milk stasis and hence increasing the risk of infections occurring.
During the process of lactation (production of milk by the breasts), the nipple and surrounding skin often swell up until the nipple is conditioned to frequent suckling by the baby. This swelling may block milk flow and thus increasing the risk of infection by bacteria such as Staphylococcus aureus which is normally present on the skin. Candida (a type of fungus) infections may also cause mastitis following the use of antibiotics. Mastitis usually causes fever as well as pain, redness and swelling of the affected breast. The presence of a lump indicates abscess formation which would normally require surgical drainage. The treatment of mastitis usually involves antibiotics with surgical drainage of abscesses if they are present.
Breast cancer
The frequency of breast cancer in women presenting with mastalgia is very low (1.2–6.7%). However, it is a serious condition which should always be ruled out.
In particular, inflammatory breast cancer (a sub-type of breast cancer) may present with a red, inflamed and painful breast. The skin may also appear dimpled or pitted like an orange peel (peau d’orange). Inflammatory breast cancer is a rare form of aggressive breast cancer that spreads along and blocks the lymph vessels in the skin of the breast. When the lymph vessels become blocked, the breast becomes red and inflamed. If there is any suspicion of breast cancer, you should consult a doctor so that he or she can carry out further investigations such as a mammogram, breast ultrasound or breast tissue biopsy (small sample of tissue removed to be studied under a microscope).
Male breast cancer is very rare and makes up less than 1% of all breast cancers. The most common symptom of male breast cancer is a breast lump, followed by breast pain and nipple discharge. Men who suffer from breast pain (mastalgia) should always consult a doctor to rule out the possibility of breast cancer.
Other medical conditions
Muscular, skeletal and mechanical problems
Muscular strain or injury may cause pain in the chest wall which can mimic breast pain. This is most commonly due to strain or injury to the pectoralis major muscle (muscle in the front of the chest) which is related to repeated use in activities such as boat-rowing or shovelling.
Spinal injury, especially in the neck and thoracic (part of body between neck and abdomen) regions, may also result in referred pain to the chest wall and mimic breast pain. In addition, a disease known as ankylosing spondylitis, a chronic inflammatory disease of the skeleton typically affecting people between 20 and 30 years of age, may also involve the chest wall and present like breast pain.
Tietze’s syndrome is another condition which can be mistaken for breast pain. It can cause sudden or long term pain and a swelling about 4 cm from the edge of the breast bone. It is due to enlargement of the cartilage around the breast bone.
Mechanical problems such as bra problems, weight changes and having large breasts may also result in breast pain.
Cardiovascular conditions
It is also possible to mistake a heart attack for breast pain. The symptoms which may be experienced by an individual suffering from a heart attack include sudden central chest pain which may spread to the left arm, increased sweating, shortness of breath and racing heart beat. This is a serious condition which requires urgent treatment. A doctor should be consulted urgently if you experience sudden central chest pain.
Abdominal/gastrointestinal conditions
Gastrointestinal conditions such as gallbladder disease, stomach ulcers and pancreatitis (inflammation of the pancreas), among others, may cause chest pain and be mistaken for breast pain. At your doctor’s office, additional investigations such as abdominal ultrasound or gastro-oesophageal endoscopy may be carried out if gastrointestinal diseases are suspected.
Impact of breast pain
Breast pain may have detrimental effects on an individual’s lifestyle. Cyclical mastalgia has been found to have a greater effect on lifestyle than non-cyclical mastalgia. The aspects of life reported to be most affected by mastalgia include sexual activity, physical activity, social activity and work/school activity.
At the doctor’s office
History
Your doctor may ask you a series of questions to determine the cause of your breast pain, including:
- Location of the pain;
- When the pain started;
- What is the pain like (sharp, dull, throbbing, radiating);
- How bad is the pain;
- What are the factors which relieve or worsen the pain;
- Timing of the pain (cyclical vs. non-cyclical, relationship with menstrual cycle);
- Associated breast symptoms (lump, nipple discharge, redness);
- Other symptoms which you may experience including fever, weight loss and loss of appetite;
- History of injury to the chest or repetitive use of the chest wall muscles;
- Menstrual history (last normal menstrual period, regularity of menstrual cycle, length of your cycle, painful periods, bleeding in between periods and pre-menstrual symptoms);
- Drug history (use of hormonal therapy, theophylline or other drugs which can cause breast pain); and
- Family history (breast cancer in particular).
Examination
It is also likely that your doctor will need to examine your breasts and the surrounding areas including the axilla (under the arms). He/she would be looking for signs such as:
- Skin changes (symmetry and contour, scars, skin retraction, dimpling, swellings, presence of ulcers and redness);
- Enlarged axillary (under the arms) or supraclavicular (above the collar bones) lymph nodes;
- Breast lumps; or
- Nipple discharge.
Investigations
At the doctor’s office, additional investigations such as imaging studies and blood tests may be required to determine the cause of breast pain or determine the type of treatment required.
Mammography
Most women who present with breast pain are under the age of 35 and therefore the role of mammography is limited. This is because mammography is less accurate in women under the age of 35 due to the breast tissue being denser in young women.
- Mammography is usually useful in certain groups of women who suffer from breast pain:
- Women older than 35 years who have not had a recent screening mammogram;
- Women younger than 35 years with abnormal findings on physical examination; or
- Women with a strong family history of breast cancer.
Ultrasound
Ultrasound is useful in detecting lumps at the site of the pain if present. It may also be used in locating abscesses if surgical drainage is required.
Treatment
Before commencing treatment for breast pain, breast diseases and other general medical conditions should be ruled out. It is important to let the doctor know about your current medications to rule out drug side effects as a cause of breast pain.
If it is found that your breast pain is due to a medication you are taking, hormonal therapy (oral contraceptive pill or hormone replacement therapy) should be decreased or discontinued if possible.
Should there be normal findings on clinical and imaging studies (that is, the breast pain is due to normal menstrual hormonal changes), the following measures may be adopted to manage physiological breast pain.
Conservative
Reassurance
Simple reassurance by the doctor that the pain is unlikely to be due to breast cancer has been proven to provide adequate relief for most women. You should, however, consult your doctor again in 6 months time should the pain persist.
Mechanical support
Precise fitting of a brassiere will provide added support for women who have large breasts and may provide pain relief. The use of a sports bra during exercise or excessive activity has been shown to provide pain reduction and superior support for the breast as measured in a study conducted by the Australian Institute of Sport.
Nutritional modifications
A low-fat diet has also been found to significantly reduce breast pain in various studies but it is thought that to derive benefit from a low-fat diet, women must decrease fat intake to less than 20% of their total daily caloric intake.
Caffeine restriction or elimination may also result in relief of breast pain. This includes avoidance of caffeine containing foods such as coffee, tea, colas and chocolate. Although the effectiveness of caffeine restriction has not been proven to be effective, it is worth considering if you have high intake of caffeine or are suffering from cyclical breast pain. It may, however, take up to 6 months before relief of symptoms are experienced after caffeine is eliminated from your diet.
Drug treatments
Paracetamol or non-steroidal inflammatory drug (NSAID)
Simple pain-relievers such as paracetamol and NSAIDs such as ibuprofen may be considered for pain relief although there are limited studies which investigate their effectiveness. The common side effects of oral NSAIDs include inflammation of the stomach wall, worsening of pre-existing asthma and sudden kidney failure.
Topical NSAIDs (used on the skin of affected areas) have also been shown to result in significant pain reduction with minimal side effects in another study.
Danazol
Danazol (sold as, for example, Danocrine) is an androgen (male sex hormone) that is effective in relieving breast pain in more than 90% of cases and is the only US FDA (Food and Drug Administration) approved drug for the treatment of cyclical breast pain secondary to hormonal changes as a result of the menstrual cycle. Side effects of danazol include increased hair growth, weight gain, voice change, increased sex drive, pain during sexual intercourse, headaches, nausea, menstrual irregularities, decreased breast size and pimple break-outs.
Selective oestrogen receptor modulators
Tamoxifen (sold as Tamosin, Genox and others) belongs to the drug class known as selective oestrogen receptor modulators which may be used for patients with severe breast pain or breast pain that is not responsive to other treatments. Tamoxifen is a drug which is more regularly used as treatment for people suffering from certain types of breast cancer.
However, tamoxifen has potentially serious side effects which includes deep venous thrombosis (blood clots developing in veins of the body most commonly in the legs and pelvic region) and an increased risk for endometrial cancer (cancer of the womb lining). Common less severe side effects include hot flushes, nausea, menstrual irregularity, dryness of the vaginal walls and weight gain.
Other agents
Bromocriptine (sold as, for example, Parlodel and Cycloset) is a long-acting dopaminergic drug that reduces prolactin (a hormone in the body which controls breast milk production) secretion by the pituitary gland (an important gland present in the brain that releases many hormones). It has been proven to improve breast pain in many women but is not as effective as danazol.
Goserelin (sold as Zoladex and other trade names) which belongs to the class of drugs known as gonadotropin-releasing hormone agonists has also been reported to be effective in up to 80% of women suffering from cyclical breast pain but may cause reduced bone density thus increasing the risk of osteoporosis with long-term use.
References
- Imgram DM, Hickling C, West L et al. A double blind randomised controlled trial of isoflavones in the treatment of cyclical mastalgia. The Breast. 2002. 11: 170-74. [Abstract]
- Ader DN and Shriver CD. Cyclical mastalgia: Prevalence and impact in an outpatient breast clinic sample. J Am Coli Surg. 1997; 185: 466-70. [Abstract]
- Murtagh J. Murtagh’s General Practice. 4th ed. New South Wales: McGraw-Hill; 2007. [Book]
- Barton MB, Elmore JG, Fletcher SW. Breast symptoms among women enrolled in a health maintenance organization: frequency, evaluation and outcome. Ann Intern Med. 1999; 130: 651. [Abstract|Full Text]
- Smith RL, Pruthi S, Fitzpatrick LA. Evaluation and management of breast pain. Mayo Clin Proc. 2004; 79: 353-72. [Abstract|Full Text]
- Symonds EM and Symonds IM. Essential obstetrics and gynaecology. 4th ed. New York: Elsevier; 2004. [Book]
- Davies EL, Cochrane A, Stansfield K et al. Is there a role for surgery in the treatment of mastalgia? The Breast. 1999; 8: 285-88. [Abstract]
- Sabel MS. Essentials of Breast Surgery. 1st ed. Philadelphia: Mosby Elsevier; 2009. [Book]
- Lucy, Armstrong, Goldman et al; Drug Information Handbook; 16th ed. [Book]
- Hindi-Alexander MC, Zielezny MA, Montes N et al. Theophylline and fibrocystic breast disease. J Allergy Clin Immunol. 1985; 75: 709-15. [Abstract]
- Peters F, Diemer P, Mecks O et al. Severity of mastalgia in relation to milk duct dilatation. Obstet Gynecol. 2003; 101:54. [Abstract]
- Tedeschi LG, Ahari S, Byrne JJ. Involutional mammary duct ectasia and periductal mastitis. The American Journal of Surgery; 106 :517-21. [Abstract]
- Department of child and adolescent health and development. Mastitis: causes and management. World Health Organisation. 2000. Available from: URL link
- National Breast Cancer Centre. Information about inflammatory breast cancer. 2007. Available online from: URL link
- Longmore M, Wilkinson IB, Turmezei T et al. Oxford handbook of clinical medicine. 7th ed. Oxford: Oxford University Press; 2007. [Book]
- Habib PA, Huang GS, Mendiola JA. Anterior chest pain: musculoskeletal considerations. Emerg Radiol. 2004; 11: 37. [Abstract]
- Kumar P and Clark M. Clinical Medicine. 6th ed. Philadelphia: Elsevier –Saunders; 2005. [Book]
- Talley NJ and O’Connor S. Clinical examination: A systematic guide to physical diagnosis. 5th ed. Australia: Elsevier; 2006. [Book]
- National Breast Cancer Centre. The investigation of a new breast symptom. [Internet]2006 [cited: 2011 Mar 15] Available from: URL link
- Burkitt HG, Quick CRG, Reed JB. Essential Surgery. 4th ed. Philadelphia: Elsevier; 2007. [Book]
- Mason BR, Page KA, Fallon K. An analysis of movement and discomfort of the female breast during exercise and the effects of breast support in three cases. J Sci Med Sport. 1000;2: 134. [Abstract]
- Gabbrielli G, Binazzi P, Scaricabarozzi I et al. Nimesulide in the treatment of mastalgia. Drugs. 1993; 46: 137-39. [Abstract]
- Colak T, Ipek T, Kanik A et al. Efficacy of topical nonsteroidal antiinflammatory drugs in mastalgia treatment. J Am Coll Surg. 2003: 196; 525-30. [Abstract]
- Lanitis S, Rice AJ, Vaughan A et al. Diagnosis and management of male breast cancer. World J Surg. 2008;32:2471-76. [Abstract]
- Jatoi I, Kaufmann M. Management of breast diseases. 1st ed New York: Springer-Verlag Berlin Heidelberg; 2010. [Book]
- Davies EL, Gateley CA, Miers M et al. The long-term course of mastalgia. J R Soc Med. 1999;91; 462-64. [Abstract|Full Text]
- Ader DN, Browne MW. Prevalence and impact of cyclic mastalgia in a United States clinic-based sample. Am J Obstet Gynecol. 1997;177:126-32. [Abstract]
- Boyd NF, McGuire V, Shannon P et al. Effect of a low-fat high-carbohydrate diet on symptoms of cyclical mastopathy. Lancet. 1988;2:128-132. [Abstract|Full Text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







