What are anticoagulants?
- How blood clotting occurs
- When are anticoagulants used?
- Anticoagulant agents
What are anticoagulants?
Anticoagulants are substances that work against (anti-) the process of blood clotting (coagulation).
How blood clotting occurs
Coagulation or blood clotting is the body’s protective mechanism against bleeding. When damage occurs to a blood vessel, a series of reactions take place involving substances known as clotting factors. They are called this because they contribute to the formation of a blood clot.
Clotting factors are normally found circulating in the blood. Most clotting factors are proteins produced by the liver that circulate in the blood in an inactive form. When one factor is activated, for example by damage to a blood vessel wall, it functions as an enzyme, activating the next clotting factor in the pathway. The final step in clotting results in the conversion of fibrinogen to fibrin. Fibrin is a protein that adheres to blood vessel walls. When activated, fibrin sticks to the blood vessel wall and traps blood cells (including platelets) as they pass, forming a mass that seals the damage in the blood vessel.
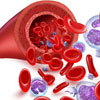 |
For more information, see Blood Function and Composition.
|
When are anticoagulants used?

Anticoagulants can be used in the treatment of several conditions, including:
- Atrial fibrillation and other arrhythmias (abnormally fast or irregular heartbeats);
- Venous thromboembolism (when a blood clot has formed in the veins);
- Prosthetic heart valves (used to replace damaged heart valves);
- After surgery (in the days/weeks following surgery, there is an increased risk of blood clots forming);
- Antiphospholipid syndrome (an autoimmune condition which predisposes individuals to form blood clots);
- Paroxysmal nocturnal haemoglobinuria (a condition in which red blood cells are destroyed, leading to anaemia and, in some cases, red urine upon waking); and
- Solid cancers (cancer is a risk factor for the formation of blood clots).
Anticoagulant agents
Currently there are two anticoagulants in use: warfarin and heparin. Both of these have certain limitations, leading to a search for new anticoagulants that are more user-friendly.
Your doctor will assess your risk of developing side effects before prescribing a medication. If you experience symptoms which appear abnormal or unusual, please tell your doctor.

Warfarin is typically used in people who require long-term anticoagulation. Its oral dosing makes warfarin ideal for this, compared with heparin which requires injection or infusion. However, warfarin has several undesirable characteristics, including:
- Therapeutic window: The range between the lowest dose that gives a good effect and the highest dose before side effects outweigh the benefits is very small;
- Dosing: The dose required to give the same effect is highly variable from person to person;
- Drug interactions: Several drugs can increase or decrease the effectiveness of warfarin; and
- Blood tests: Tests to measure the body’s ability to clot blood (prothrombin time), measured as the international normalised ratio (INR), are required regularly.
On beginning warfarin therapy, a blood test to measure INR occurs on a daily basis until the target INR has been achieved and maintained for at least two consecutive days. Monitoring then occurs every 2–3 days for the next few weeks, and then with decreasing frequency depending on the stability of the results. If the INR remains stable, laboratory testing can take place a minimum of every 4 weeks.
The three most common reasons for requiring warfarin therapy are:
- Atrial fibrillation;
- Venous thromboembolism; and
- Prosthetic heart valves.
The main side effect of warfarin use is bleeding. This risk is increased when the INR is above the recommended value for you. If any of the following apply to you, you must speak with your doctor immediately as you should not be taking warfarin:
- Recent haemorrhage;
- High falls risk;
- Inability to have INR determination;
- Pregnancy;
- Hearing or vision impairments, or difficulties with numeracy, in people required to listen to dose alterations and carry them out without the aid of a carer.
The primary use of heparin is to prevent the formation or progression of thromboembolism (formation of blood clots within the blood vessels that may break off to block blood vessels at other sites). Heparin acts very soon after entering the body, so it is ideal for people who require rapid or short-term anticoagulation (e.g. after surgery).
There is an increased risk of blood clots forming after surgery for two reasons:
- The operation may result in a large amount of trauma to many blood vessels and tissues; and
- Post-operative pain often leads to reduced mobility, so the leg muscles, which normally act as pumps returning blood to the heart, are no longer employed and the blood within the veins is said to be still (venous stasis).
Heparin is also commonly used in the initiation of warfarin therapy, to provide anticoagulation until the INR is therapeutic. In this case, heparin is given at the same time as warfarin for at least four days. Once the INR is within the therapeutic range on two occasions, at least 24 hours apart, the heparin can be discontinued. Doing this may also reduce the risk of experiencing some of the side effects of warfarin.
Heparin is a relatively safe alternative to warfarin where anticoagulation is indicated in pregnancy. As with all medications to be used during pregnancy, it should first be discussed with your doctor.
The main side effects associated with heparin use include:
- Bleeding;
- Low platelet levels; and/or
- Heparin-induced osteoporosis.
An antidote is available for some forms of heparin. Where excess bleeding occurs (the main side effect of anticoagulants) such as large bruises and blood loss from the nose, mouth or anus, protamine can be injected into the veins. Protamine, a protein derived from fish sperm, binds to heparin and inactivates it. By inactivating the heparin, the bleeding tendency is reduced and the bleeding is more easily controlled.

Newly-developed anticoagulants have been designed to target specific enzymes or steps in the coagulation pathway. While some are available for oral use, the majority of these new anticoagulants require injection or infusion like heparin.
Currently in Australia, the newer anticoagulants require further evaluation and are only being used for research purposes. Potentially, these newer agents will be at least as effective as the already-available anticoagulants, without the need for ongoing monitoring.
References
- Saladin KS. Anatomy and Physiology: A Unity of Form and Function (3rd edition). Boston: McGraw-Hill; 2004. [Publisher]
- Tadros R, Shakib S. Warfarin: Indications, risks and drug interactions. Aust Fam Physician. 2010;39(6):476-9. [Abstract | Full text]
- Baglin TP, Keeling DM, Watson HG. Guidelines on oral anticoagulation (warfarin): Third edition – 2005 update. Br J Haematol. 2006;132(3):277-85. [Abstract | Full text]
- Hirsh J, O’Donnell M, Weitz JI. New anticoagulants. Blood. 2005;105(2):453-63. [Abstract | Full text]
- Gallus A. New oral anticoagulants: Clinical applications. Aust Prescr. 2010;33(2):42-7. [Full text]
- Anticoagulants, antithrombotics. In: MIMS 2008;45(6). St Leonards, NSW: MIMS Australia; 88-90. [Publisher]
- Ansell J, Hirsh J, Poller L, et al. The pharmacology and management of the vitamin K antagonists: The Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest. 2004;126(3 Suppl):204S-233S. [Abstract | Full text]
- Ansell J, Hirsh J, Dalen J, et al. Managing oral anticoagulant therapy. Chest. 2001;119(1 Suppl):22S-38S. [Full text]
- Hirsh J, Raschke R. Heparin and low-molecular-weight heparin: The Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest. 2004;126(3 Suppl):188S-203S. [Abstract | Full text]
- Wessler S, Gitel SN. Heparin: New concepts relevant to clinical use. Blood. 1979;53(4):525-44. [Full text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.








