- Introduction to alcohol and pain
- Alcohol and mechanism of action
- Suggestions for pain and alcohol treatment
- Studies on chronic pain patients and alcohol
Introduction to alcohol and pain

Pain signals are then carried along nerves to the spinal cord, transmitted upwards and perceived by various parts of the brain. This is called nociceptive pain. In chronic pain sufferers, there is also a type of pain known as neuropathic pain.
Neuropathic pain is experienced when the nervous system is damaged or not working properly. Treatment of pain has been an important issue in all medical systems. For many years, analgesic (pain relieving) substances have been intensively studied and sought out. Alcohol was among the earliest substances found to be effective. Over 80% of the population drink alcohol.
Alcohol and mechanism of action
In everyday life, many people continue to deal with pain by self-medicating with alcohol. Due to its ability to depress the central nervous system (CNS), it slows down the brain and nervous system, and delivers a certain amount of pain relief. It also has muscle relaxant and sedating properties.
Unfortunately, there is a tendency for alcohol to be abused (alcohol abuse and alcoholism), and the use of alcohol for pain relief can easily cause problems. It is not uncommon for the amount of alcohol used to become excessive. If combined with the wrong medications, alcohol can have an additional lowering (depressant) effect on the nervous system, leading to disastrous consequences.
With prolonged use and excess consumption, the body begins to build up a tolerance to the effects of alcohol. It takes more alcohol to produce the same results. Increased amounts of alcohol over time can cause many health problems, affecting all organ systems in the body. This includes problems such as impaired brain function and memory, to peptic ulcers and liver cirrhosis. In addition, because alcohol is a major depressant, it will exacerbate any underlying depression and is also dangerously habit-forming (addictive). Alcohol may provide temporary relief of pain, but may worsen the problems that pain sufferers may face.
Suggestions for pain and alcohol treatment

- Ask patients with pain about alcohol use;
- Ask patients with drinking problems about pain;
- Educate patients about the risks of using alcohol as a pain reliever;
- Promote other more safer, more effective methods of pain relief.
Studies on chronic pain patients and alcohol
In our older population, many people suffer from pain and a large number of people drink alcohol excessively. There have been some studies performed, to examine the relationship between pain and alcohol problems amongst older adults. 401 adults living within the community were studied over a three year period.
At the beginning of the study, more of the problem drinkers (people who drank too much alcohol) than non-problem drinkers reported having moderate to very severe pain (43% versus 30%). A greater proportion of problem drinkers used alcohol to treat their pain (38% versus 14%).
Results from the study show that the level use of alcohol to manage pain predicted:
- an increase amount of chronic health problems and injuries in men
- more drinking problems in women after three years.
In conclusion, whilst alcohol is used to self medicate and manage pain, there are many problems with it’s use. Large doses may seem to help temporarily, but more effective, safe and long term pain killers should be used to provide relief from pain.
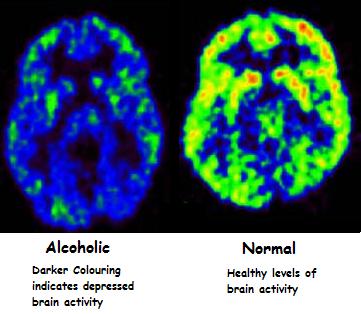
The image below is that of activity levels in an alcoholic’s brain compared to a healthy person’s brain.
More information
 |
For more information on drinking alcohol, including drinking disorders and alcohol’s effect on the body, as well as some useful tools, see Alcohol. |
References
- Brennan PL, Schutte KK, Moos RH. Pain and use of alcohol to manage pain: prevalence and 3-year outcomes among older problem and non-problem drinkers. Addiction. 2005;100(6):777-86. [Abstract]
- Hanson RW. Biophysical aspects of pain [online]. 2003 [cited 2 April 2006]. Available from: URL link
- Rang HP, Dale MM, Ritter JM. Pharmacology. China: Churchill Livingstone; 2000. [Publisher]
- Sadock B, Sadock V. Pocket Handbook of Clinical Psychiatry. USA: Lippincott Williams & Wilkins; 2001. [Publisher]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







