Why is rehabilitation after prostate cancer treatment important?
- Urinary incontinence
- Erectile dysfunction
- Urinary incontinence and erectile dysfunction
- Emotional support and counselling
Why is rehabilitation after prostate cancer treatment important?
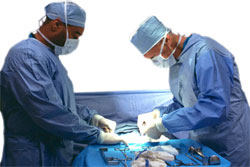
Prostate cancer is one of the most commonly treated malignancies in Western society. Attempts at curing prostate cancer may involve surgery, radiotherapy or high intensity focused ultrasound. The aims of any prostate cancer treatment are to achieve cure of the cancer, preserve urinary control and preserve erectile function. Unfortunately, and notwithstanding increasing treatment sophistication and therapeutic diligence, very significant side effects are associated with prostate cancer therapy, especially with regards to urinary incontinence and erectile dysfunction.
During the recovery period after prostate cancer treatment, patients are offered a comprehensive rehabilitation plan, including appropriate emotional and psychological support. The preferred approach is multi-disciplinary, involving a urologist, a physiotherapist experienced in the management of male urinary incontinence, and a psychologist adept at couples, cancer and sexual dysfunction counselling.
Urinary incontinence

Intensive pelvic floor training
It is normal for the majority of men to experience a degree of sphincter weakness incontinence once the urinary catheter is removed. A physiotherapist can instruct these men in the correct technique for pelvic floor training. Correct instruction is very important, as those not taught the proper technique tend to strain abdominally in an inappropriate fashion. With daily training, many men will regain bladder control within three months.
The male sling is appropriate for men with mild to moderate stress urinary incontinence that has not responded to conservative measures. The sling is a polypropylene mesh material that is inserted via a small perineal incision. The patient is operated on a day stay basis.
For cases of moderate to severe urinary incontinence, the inflatable artificial urinary sphincter is the standard of care. The artificial urinary sphincter is constructed of biocompatible silicon and is primed with a normal saline solution. It consists of a reservoir of fluid placed intra-abdominally, an inflatable and deflatable cuff that surrounds the urethra and a deflate mechanism that is situated beneath the scrotal skin. The artificial sphincter is inserted via a small transverse scrotal incision and the patient discharged after an overnight stay in hospital. After a six week settling in period the device is activated and the patient taught the simple technique of manipulating the small scrotal pump to relax the cuff in order to facilitate voiding.
In difficult cases involving urethral fibrosis such as after external beam radiotherapy, a double cuff system may be implanted to ensure restoration of urinary control.
Radio-fibrotic urethral stricture disease may occur with either external beam radiotherapy or with brachytherapy. Should these strictures not respond to urethrotomy or stricture incision, a urethral prosthesis may be endoscopically placed in an attempt to allow urethral healing without stricturing.
Erectile dysfunction
Similarly, 50% of pre-treatment potent men have significant erectile dysfunction at two years after radiotherapeutic intervention. This erectile dysfunction is due to corporal fibrosis of the erectile tissue.
It is very important that penile injection therapy be commenced four to six weeks following radical prostatectomy surgery. The patient is taught by an experienced nurse the technique of self injection into the side of the penis. Vaso-active combinations of drugs are used, most commonly combinations of prostaglandin, papaverine and phentolamine. Early introduction of penile injection therapy after surgery is critical in order to prevent permanent atrophy of the erectile mechanism. Appropriate warnings are given to the patient in order that priapism prevented, and if it occurs treated promptly.
PDE-5 inhibitors will only work when a degree of cavernosal nerve function exists. For men who have had successful cavernosal nerve preservation, it is frequently the case that due to neurapraxia the nerves do not function even partially for at least three months. It is therefore appropriate to introduce oral therapy for erectile dysfunction at three months post operatively. These compounds are safe, the absolute contraindication to their use is in combination with nitrate compounds.
The implantation of an implantable penile prosthesis is the gold standard in terms of permanent restoration of quality erectile function. Should the patient be impotent pre-operatively or should potency not return post-operatively the patient should be counselled with respect to penile prosthetic surgery in terms of adequate long-term management.
The inflatable penile prosthesis is inserted through a small transverse incision and comprises and intra abdominal reservoir of normal saline, inflatable cylinders within the penis and an inflate and deflate pump mechanism located within the scrotum. Surgery is performed on a twenty-four hour hospital stay basis. The great popularity of the penile prosthesis is the restoration of spontaneous and therefore romantic lovemaking as well as elimination of performance anxiety.
Urinary incontinence and erectile dysfunction

Emotional support and counselling
The prostate cancer patient and his partner are suddenly forced to deal with a number of very major life stresses. There is the diagnosis of cancer, the prospect of radical surgery or radiotherapy, the fear of urinary incontinence and the concern about ongoing erectile function. These concerns are best anticipated and dealt with in a multi-disciplinary approach involving a partnership between the patient, his partner, the urologist, physiotherapist and psychologist. In this way successful rehabilitation of the patient to a normal quality life is assured.
(Article kindly contributed by Dr P M Katelaris, Consultant Urologist, Director Prostate Cancer Foundation of Australia, Director Prostate Cancer Research Division of the Institute of Magnetic Resonance Research, and Director of the Prostate Cancer Rehabilitation Centre.)
More information
 |
For more information on prostate cancer, including diagnoses, types of treatments, and some useful tools, videos and animations, see Prostate Cancer. |
References
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.








