- Introduction
- Psoriasis Vulgaris
- Flexural/Inverse Psoriasis
- Guttate Psoriasis
- Erythrodermic Psoriasis
- Generalised Pustular Psoriasis
- Palmoplantar Psoriasis
- Scalp Psoriasis
- Nail Psoriasis
Introduction
Psoriasis is a disease which affects multiple systems within the body, predominantly the skin and the joints. Skin disease which can present in multiple different ways and degrees of severity is the hallmark of psoriasis. The severity of psoriasis is defined in terms of how much body surface area and which body parts are involved. When the hands, feet, face and/or genital regions are involved, the impact on the individual and how they go about their daily activities is more significant.
It is well established that there are different types of psoriasis with psoriasis vulgaris being the most common form. Other subtypes include flexural psoriasis, guttate psoriasis, erythrodermic psoriasis, generalised pustular psoriasis, palmoplantar psoriasis in addition to psoriasis that involves certain body sites including the scalp and nails.
Your treating doctor will establish the best treatment plan for your psoriasis based on your age, your type of psoriasis, the site and extent of skin involvement, any previous treatment you may have had and any other medical problems you may have.
 |
For more information about the causes of psoriasis, incidence statistics, predisposing factors and more, see Psoriasis. |
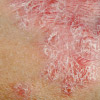
Psoriasis vulgaris
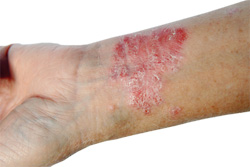
Psoriasis vulgaris either has an early onset occurring at a mean age of 5 years or a late onset presenting around 22 years of age. Those with disease that presents early typically have a longer and more severe course and often have other family members with psoriasis. Psoriasis occurs at equal rates for both males and females. Certain population groups including West Africans, Japanese, Inuits and the American Indians have very low rates of psoriasis vulgaris.
There are several treatment options available for the treatment of psoriasis vulgaris, based on the severity of disease and extent of skin involvement. For mild to moderate disease, treatment options include corticosteroid creams applied to the skin (including hydrocortisone and mometasone), vitamin D analogues or oral retinoids (acitretin). Where the disease is more extensive or associated with disfigurement or disability, phototherapy, systemic therapy or biological therapy (e.g. adalimumab (Humira), ustekinumab (Stelara)) are indicated.
 |
For more information on the different types of treatments available for psoriasis and how effective they are, see Treatment Options for Psoriasis. |
Flexural/Inverse Psoriasis
Inverse psoriasis is a rare form of psoriasis which is also known as flexural or intertriginous psoriasis. This subtype of psoriasis can occur in any area where two skin surfaces meet. Classically the skin of the groin region, armpits and genitals are affected. In these regions the skin appears red, shiny, and moist, with clear borders, and can sometimes crack in the centre.
This rare form of psoriasis accounts for 3–7% of people with psoriasis. A small Chinese study found that the average age of onset for inverse psoriasis is 28.9 years. Occasionally people with another subtype of psoriasis known as pustular psoriasis go on to develop inverse psoriasis.
Recent guidelines from the National Psoriasis Foundation recommend the use of low to moderate strength corticosteroids for flare ups of this type of psoriasis and calcipotriene and either tacrolimus or pimecrolimus (e.g. Elidel) for treatment of inverse psoriasis in the long term.
 |
For more information on the different types of treatments available for psoriasis and how effective they are, see Treatment Options for Psoriasis. |
Guttate Psoriasis

This type of psoriasis accounts for about 2% of individuals with psoriasis. One-third of people with guttate psoriasis will develop psoriasis vulgaris at some point. Guttate psoriasis classically affects children and young adults. It is strongly associated with a bacterium called streptococcus and typically occurs 1–2 weeks after an episode of tonsillitis caused by this bacterium. Guttate psoriasis can resolve if left untreated but can also recur.
Current research is limited in identifying the best treatment for guttate psoriasis. Commonly used regimens include topical tar and UVB phototherapy, anthralin and topical corticosteroids, psoralen in combination with ultraviolet A (PUVA) and more recently vitamin D analogues. Many dermatologists recommend the use of antibiotics to treat associated tonsil infection and may recommend an operation to remove the tonsils if attacks are recurrent.
 |
For more information on the different types of treatments available for psoriasis and how effective they are, see Treatment Options for Psoriasis. |
Erythrodermic Psoriasis
Erythrodermic psoriasis is a severe form of psoriasis that affects greater than 75% of the skin. This type of psoriasis can present with involvement of the skin, hair loss or breakdown of the finger or toe nails. At its extreme it is associated with fever, chills, fatigue, failure of the heart and whole body infection due to a bacterium which can affect the skin known as staphylococcus aureus (also known as Golden Staph). Some people will present with a rapid onset of disease that requires aggressive treatment whereas others experience a more benign course with chronic frequent relapses.
This subtype of psoriasis is extremely rare affecting approximately 1–2.5% of people with psoriasis. Erythrodermic psoriasis can arise in people with long term psoriasis vulgaris or it can occur as the initial presentation of psoriasis.
The medical literature lacks clear guidelines as to the best treatment for erythrodermic psoriasis. Cyclosporin and infliximab are the most rapidly acting agents with acitretin (e.g. Neotigason) and methotrexate (e.g. Methoblastin, Methotrexate Kabi) being other appropriate options which work more slowly. Second line treatment with etanercept (e.g. Enbrel) or combination therapy may be considered by your doctor. It is important to also avoid therapies which may exacerbate this condition including oral steroids and phototherapy.
 |
For more information on the different types of treatments available for psoriasis and how effective they are, see Treatment Options for Psoriasis. |
Generalised Pustular Psoriasis

Factors which appear to trigger GPP include infections, corticosteroids, pregnancy and certain medications. GPP appears in two distinct groups of individuals. The first group includes those who have previously had psoriasis vulgaris and this group typically gets GPP later in life, usually after treatment with steroids. The second group has no history of psoriasis and tends to develop GPP at an earlier age, typically after an infection.
People with GPP are usually quite unwell and require admission to hospital. Rapid resolution of the blistering lesions is best achieved with oral retinoids (e.g. Zorac, Neotigason). Other treatment will be directed by the treating doctor and may include intravenous antibiotics to prevent further infection, measures to achieve normal body temperature, antiseptic baths and, rarely, measures to maintain normal heart function.
 |
For more information on the different types of treatments available for psoriasis and how effective they are, see Treatment Options for Psoriasis.. |
Palmoplantar Psoriasis
Palmoplantar pustulosis is a chronic form of psoriasis which tends to come and go. As the name suggests it affects the palms of the hands and the soles of the feet. The individual normally experiences stinging and burning of the affected area/s which are often itchy. Typical blisters are 2–5 mm in diameter and yellow and then evolve into dusky-red spots with a scab.
Palmoplantar pustulosis is more common in females and typically occurs between the age of 50 and 60 years. It tends to persist for years with a pattern of recurrent episodes. Individuals with this type of psoriasis are at increased risk of developing psoriasis vulgaris.
 |
For more information on the different types of treatments available for psoriasis and how effective they are, see Treatment Options for Psoriasis. |
Scalp Psoriasis

Treatment of scalp psoriasis is best directed by your treating doctor. Mild disease is best treated with shampoos containing either tar or ketoconazole followed by the application of corticosteroid lotion. Where disease is more severe the initial focus is to soften the plaques using salicylic acid in mineral oil and leaving this on the scalp overnight covered by a shower cap. Once the plaques have softened, fluocinolone cream or lotion can be applied and again left in overnight with a shower cap. Clobetasol propionate or calcipotriene lotions are then used to stop the plaques from reappearing. If these measures are not successful, your treating doctor may wish to consider systemic treatment.
 |
For more information on the different types of treatments available for psoriasis and how effective they are, see Treatment Options for Psoriasis. |
Nail Psoriasis
Involvement of the nail can occur in all psoriasis subtypes. Fingernails are affected in 50% of cases of psoriasis and toenails in 35%. The most common abnormality is that of pitting or indentations of the nail itself. Localised colour changes known as “oil drop spots” are characteristic and occur when white blood cells are present beneath the nail itself. Severe psoriatic involvement of the nails can result in thickened nails and onychodystrophy. If the entire nail is affected a white, crumbly, poorly adherent nail can be seen. Pustular psoriasis can cause the formation of pustules under the nail bed, which can result in the loss of the entire nail.
Treatments applied to the nail in the form of creams or lotions are generally not effective. The most successful treatments include PUVA application, systemic retinoids and other systemic agents including methotrexate and cyclosporine. The focus of treatment is to restore normal growth of the nail.
 |
For more information on the different types of treatments available for psoriasis and how effective they are, see Treatment Options for Psoriasis. |
References
- Menter A, Korman A, Elmets C, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. Section 6: Guidelines of care for the treatment of psoriasis and psoriatic arthritis: case-based presentations and evidence based conclusions. Journal of the American Academy of Dermatology. 2011; 65: 137-174. [Abstract]
- Murphy G, Reich K. In touch with psoriasis: topical treatments and current guidelines. Journal of the European Academy of Dermatology and Venereology. 2011; 25: 3-8. [Abstract Full Text]
- Wolff K, Johnson R. Fitzpatrick’s Colour Atlas and Synopsis of Clinical Dermatology (6th edition). New York: McGraw Hill Medical; 2009. [Publisher]
- Luba K, Stulberg D. Chronic Plaque Psoriasis. American Family Physician. 2006; 73: 636-639. [Full Text]
- Green L. An overview and update on psoriasis. Nursing Standard. 2011; 25: 47-55. [Abstract]
- Syed Z, Khachemoune A. Inverse Psoriasis: case presentation and review. American Journal of Clinical Dermatology. 2011; 12: 143-146. [Abstract]
- Wang G, Chunying L, Tianwen G et al. Clinical analysis of 48 cases of inverse psoriasis: a hospital based study. European Journal of Dermatology. 2005; 15: 176-178. [Abstract]
- Kulb R, Bagel J, Korman N et al. Treatment of intertriginous psoriasis from the medical board of the National Psoriasis Foundation. J Am Acad Dermatol. 2009; 60: 120-124. [Abstract]
- Chalmers R, O’Sullivan T, Owen C. A systematic review of treatments for guttate psoriasis. British Journal of Dermatology. 2001; 145: 891-894. [Abstract]
- Parnham M, Bruinvels J (Eds): Treatment of psoriasis. Basel: Birkhauser Verlag. 2008. [Publisher]
- Rosenbach M, Hsu S, Korman N et al. Treatment of erythrodermic psoriasis: From the medical board of the National Psoriasis Foundation. Journal of American Academy of Dermatology. 2010; 62: 655-662. [Abstract]
- Iizuka H, Takahashi H, Ishida-Yamamoto. Pathophysiology of generalised pustular psoriasis. Archives of Dermatological Research. 2003; 295: S55-S59. [Abstract]
- Therapeutic Guidelines. Psoriasis. Revised February 2009. Available from URL Link
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







