- What is male circumcision?
- History of male circumcision
- The foreskin
- Prevalence of male circumcision
- Why parents or men might choose to circumcise
- Health benefits of circumcision
- Limitations and health risks associated with male circumcision
- Ethical considerations surrounding male circumcision
What is male circumcision?
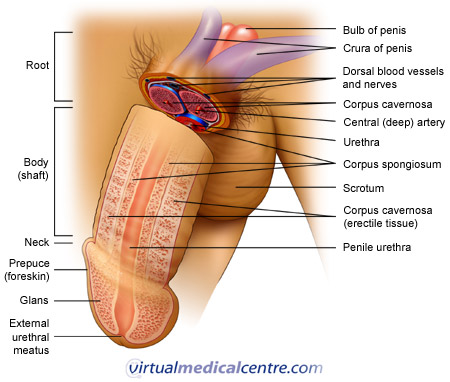
Male circumcision is a surgical procedure which involves the removal of the foreskin (also known as the prepuce) of the penis. The foreskin is a shaft of skin which covers the head of the penis (glans penis). In an adult male the foreskin can be retracted for cleaning purposes. It also retracts naturally during sexual intercourse.
Circumcision is a very common and relatively simple surgical procedure, which can be performed using a number of methods. However like all surgery, circumcision carries risks, including haemorrhage, infection and pain. These complications can be serious (e.g. penile amputation) and even cause death.
Although circumcision has been performed for cultural and religious reasons for thousands of years, most professional medical associations oppose routine neonatal circumcision (and particularly circumcision without anaesthesia), and recommend the procedure only in cases where there are clearly defined medical reasons.
Many of the health benefits once purported to be associated with circumcision (e.g. reduced masturbation) are now highly questionable. The proven health benefits of circumcision are typically minor (e.g. reduced risk of urinary tract infection) and the conditions are often prevented by other, less invasive measures and/or treated simply with antibiotics. The exception is human immunodeficiency virus (HIV), and circumcision has been recommended as an HIV prevention measure in countries where the virus is highly prevalent such as sub-Saharan Africa. However as HIV prevalence is relatively low in Australia, widespread circumcision could not be justified for HIV prevention purposes. In Australia circumcision for health or medical purposes is recommended for only a few, relatively rare indications.
Circumcision is performed for personal, cultural and/or religious reasons by a range of cultural groups. For example, amongst Jews and Muslims, the practice is almost universal. Many families in which the father is circumcised, have the male sons circumcised so they will look like the father, or simply because the father is circumcised.
There are numerous ethical considerations relating to the human rights of the child and the rights of parents (for example freedom of religious expression), which must be considered when deciding whether or not a child should be circumcised. Medical practitioners can provide parents who are considering having their child circumcised, and adult men considering undergoing the procedure, objective information about the health risks and benefits. Once they have received and understood this information, adults or parents who decide to have their child circumcised must sign a consent form before circumcision can be performed.
History of male circumcision
In Western medicine, male circumcision gained popularity in the late 19th and early 20th century. At that time, neonatal circumcision without anaesthesia was performed routinely in a number of Western countries, including Australia. While religious values played a role in some circumcisions, for the most part the procedure was performed for spurious medical reasons. Masturbation, cancer and mental disorders were amongst the diseases circumcision was purported to protect against at the time. Circumcision may also have been performed to show social status; because revered men were circumcised, circumcision was seen as an indicator of one’s position in society.
Medical support for routine male circumcision began to decline in the second half of the 20th century. The Australian Paediatric Association adopted an anti-circumcision policy in 1971. Rates of neonatal and infant circumcision declined in Australia thereafter. While the Australian Paediatric Association and other professional bodies in Australia have continued to review scientific evidence of the relative health risks and benefits of male circumcision since that time, they maintain that there is no medical indication for the routine circumcision of male neonates. Routine circumcision is not currently covered by Medicare in Australia.
The foreskin
What is the foreskin?
The foreskin (or prepuce) is a fold of penile skin which covers the head (glans) of the penis. It consists of an outer skin and an inner mucosa. The foreskin typically appears in the male foetus after some eight weeks of growth and fully covers the glans penis by 16 weeks of foetal growth. At birth the foreskin is fully developed, however it has rarely separated from the glans penis, and thus cannot be retracted. Separation occurs spontaneously during childhood, usually before five years of age. As the foreskin separates from the glans, dead skin cells with a white “cheesy” appearance known as smegma, collect between the layers of skin. The accumulation of smegma is normal and assists the separation process, however it may also result in inflammation of the glans and/or foreskin. By puberty the foreskin is fully retractable and can be pulled away from the glans penis.
Purpose of the foreskin
Protective functions
The foreskin protects the glans penis, urethral meatus and inner preputial epithelium in a similar way to which the eyelids protect the eyes. When the penis is not erect, the foreskin fully covers these sections of the penis, and thus reduces irritation and the possibility of contamination. The preputial sac (the space between the penis and the foreskin when the foreskin is in place), remains moist due to secretions from the prostate, urethral glands and seminal vesicle.
The foreskin further plays a role in the immune system, however similar to the role of the foreskin in sexual function, the foreskin’s immunological role remains poorly understood by medical practitioners.
Sexual functions
The foreskin is highly responsive to sexual stimulation and plays an important role in male sexual function. Most obviously the foreskin provides adequate skin to enable the penis to expand during erection (at which time the foreskin naturally retracts). The foreskin contains many sensitive nerves and thus also has an erogenous function, however the extent to which sexual sensations differ between circumcised and uncircumcised men is currently poorly understood. The natural moisture of the preputial sac also acts as a lubricant to reduce friction during sexual penetration.
Removal of the foreskin almost certainly changes sexual function and sensation, however there is conflicting evidence regarding the nature and direction of those changes. While in theory one would expect reduced sexual sensation and functions following the removal of a highly erogenous tissue, in practice, circumcised and uncircumcised men appear to have similar sexual responses.
Foreskin hygiene
During infancy, when the foreskin remains attached to the glans, no special hygiene practices are needed. Rather the foreskin should be left alone as attempts to retract it for cleaning may result in pain.
Following separation of the glans and foreskin during childhood, the foreskin should be retracted and cleaned in the shower or bath. Once cleaning is complete, the foreskin should be replaced over the glans, to prevent swelling and irritation.
Circumcision is sometimes promoted as a penile hygiene measure, however there is no evidence of an association between penile hygiene and circumcision status. None the less, cleaning the foreskin is an important hygiene measure and one study showed it reduced the risk of inflammatory conditions of the penis and phimosis.
Prevalence of male circumcision

In Australia, it is estimated that 10-20% of the male population are circumcised in infancy. More than half (59%) of the adult men living in Australia are circumcised as are 69% of those that were born in Australia. Circumcision is less prevalent amongst younger men, under 20 years of age, of whom 32% are circumcised.
Why parents or men might choose to circumcise
Circumcision may be carried out for religious, cultural, medical or personal reasons.
Medical
Professional associations throughout the Western world (e.g. the Australian Association of Paediatricians) typically oppose circumcision as a preventative health measure. The health conditions associated with the foreskin are either rare or easily treated in developed countries, and thus the health benefits of circumcision do not justify the risk of the procedure. In Australia, there are only a few, fairly rare medical indications for circumcision and in practice circumcision is typically conducted for non-medical reasons.
Religious or cultural
A number of religious groups perform male circumcision, most prominently Jews and Muslims, amongst whom the practice is almost universal. In many African cultures, circumcision is also performed for religious/cultural reasons, usually as part of a coming of age ceremony. In these cases circumcision signifies manhood and sexual initiation. In African settings, the procedure is usually performed without anaesthetic, and often without basic hygiene precautions (e.g. sanitising or using new cutting implements for each boy’s procedure). Under these conditions the surgery is extremely dangerous and death is common.
Personal
In Western countries where circumcision is widespread, parents may chose to have their male sons circumcised in order to carry on a family tradition, or so that the boys look the same as their fathers. Adult men may choose to be circumcised for aesthetic reasons.
Health benefits of circumcision

Human papilloma virus and cancer of the penis and cervix
Human papilloma virus
It is now well established that certain sub-types of the human papilloma virus (HPV) are the causal agents in penile and cervical cancers. Circumcision has been thought to reduce the risk of infection with HPV and thus scientists have hypothesised that circumcision may also prevent penile cancer in circumcised men and cervical cancer in their female partners.
Available scientific evidence demonstrates that circumcised men are less likely to contract HPV than uncircumcised men. For example, a study in which data from seven separate studies on circumcision and HPV were combined for analysis, reported lower rates of HPV infection in circumcised men (5.5%) compared to uncircumcised men (19.6%). That study reported that circumcised men were 63% less likely to be HPV infected.
Penile cancer
There is strong evidence that neonatal circumcision reduces the risk of penile cancer, however circumcision later in life has not been shown to do so. Estimates suggest that circumcised men are at least ten times less likely to develop penile cancer and virtually all cases of penile cancer occur in men who were not circumcised at birth. While the evidence is strong, penile cancer is such a rare condition (i.e. occurring in less than 1:100,000 men), that routine neonatal circumcision cannot be justified to reduce penile cancer incidence alone.
Cervical cancer
In relation to cervical cancer, the best available evidence suggests that circumcision protects the female partners of circumcised men. The monogamous partners of men who have a high risk of contracting HPV (men with more than six sexual partners) particularly benefit from circumcision. These women are 58% less likely to develop cancer of the cervix than their counterparts who are in monogamous sexual relationships with uncircumcised men.
Urinary tract infection
Recent large studies of associations between circumcision and urinary tract infection in boys reported that circumcised boys were 87% less likely than their uncircumcised counterparts to develop urinary tract infections. Other previous studies have shown similar results for infants, boys and adult men.
However, as urinary tract infections are minor conditions, occur relatively infrequently (boys have about a 1% chance of developing a urinary tract infection) and are easily treated with antibiotics, circumcision to prevent urinary tract infection is not justifiable. The Royal Australasian College of Physicians note that the likelihood of circumcision complications (~2%) far outweighs any benefit from reduction in urinary tract infections.
Sexually transmitted infections
The association between male circumcision and the risk of sexually transmitted infection (STI) varies depending on the specific STI. There is strong evidence that circumcision protects against HIV and good evidence that it protects against ulcerative STIs, particularly syphilis and chancroid. Evidence for other STIs is less conclusive, and more research is needed to determine whether or not circumcision protects against these STIs.
In Australia, there is no association between circumcision status and self reported incidence of most STIs at the population level. The exception is candidiasis (thrush), an infection which occurs on the foreskin, and may occur as a result of sexual exposure or for other reasons. The Australian Association of Paediatric Surgeons do not support circumcision as an STI prevention strategy and recommend that sexually active individuals take other precautions to reduce the risk of HIV infection (e.g. wearing a condom).
HIV
Circumcision received increasing attention as an HIV prevention intervention in the 21st century. Three large studies conducted in Africa showed that heterosexually active circumcised men were at least 50% less likely to contract HIV than their uncircumcised counterparts.
The foreskin of the penis contains a high concentration of cells called Langerhans’ cells. These cells assist HIV to enter an uninfected man’s body and the foreskin is therefore thought to be the primary penile entry point for HIV. Removal of the foreskin is thought to reduce the ability of HIV to infect the penis. Male circumcision is now being recommended as an HIV prevention intervention in countries where HIV is highly prevalent, circumcision rates are low and HIV is predominately transmitted heterosexually.
There is insufficient evidence to determine whether or not circumcision protects men against HIV during anal sex.
In Australia where HIV prevalence at a population level remains low, and the majority of HIV infections occur amongst homosexually active men, circumcision is not justified as an HIV prevention intervention. Rather, sexually active individuals should take other precautions, for example use condoms to reduce the risk of HIV infection.
There is no evidence that the female partners of circumcised men have a lower risk of HIV infection.
Syphilis and chancroid
There is good evidence that circumcision protects against syphilis and reduces the risk of chancroid. Available evidence shows that circumcised men were 33% less likely to contract syphilis than uncircumcised men. The majority of studies which have examined associations between circumcision and chancroid have also reported that circumcised men are less likely to contract the infection than uncircumcised men.
Herpes simples virus type 2 or genital herpes
Current evidence suggests that there is an association between circumcision status and herpes simples virus type 2 (HSV-2) infection. Analysis of data from ten studies on this topic showed that circumcised men are at least 12% less likely than uncircumcised men to become infected with HSV-2.
Other STIs
There is currently insufficient evidence to determine whether circumcision influences the risk of contracting gonorrhoea, Chlamydia, non-gonococcal urethritis and other types of urethritis or genital warts.
Limitations and health risks associated with male circumcision

Health risks
The surgical risks of circumcision are typically minor and involve bleeding, infection and pain. When circumcision is conducted by a professional in appropriate sanitary conditions, complications occur in 1-5% of cases. However, it is important to note that more serious complications, such as meningitis and septicaemia can occur as a result of the surgery, and these conditions can lead to death. There have also been cases of penile amputation resulting from circumcision complications.
Circumcision in unhygienic conditions, for example as part of a coming of age ceremony, incurs substantial risk. In countries like South Africa, where circumcision is still practiced amongst some ethnic groups using traditional surgical techniques, death and serious cases of infection occur each year as a result of the procedure.
Psychological risks
There have been claims that male circumcision has adverse psychological effects, however there is no scientific evidence to support these claims.
Sexual function and practice
Some opponents of male circumcision claim that removal of the foreskin interferes with sexual satisfaction or performance. There is no scientific evidence to support this claim, although there have been a few studies of the role of the foreskin in male sexual pleasure.
Available evidence for Australia comes from a study of the sexual practices and experiences of Australian men. That study found no significant differences between circumcised and uncircumcised men in terms of masturbation or sexual practices at last sexual encounter. It also reported no significant differences in reported sexual pleasure or time to reach orgasm between the two groups, but the study did not examine penile sensitivity directly.
Contrary to claims that circumcision causes sexual dysfunction, uncircumcised men in the Australia study, were more likely to report difficulty maintaining an erection and pain during sexual intercourse, than circumcised men. This was true even after confounding factors such as age were considered. The study did not examine why such differences were apparent, and highlighted that it may be as a result of psychological or physiological reasons, rather than a direct result of circumcision status.
With regards to the sexual satisfaction of a man’s sexual partners, there is some evidence which suggests that circumcision may be more satisfactory to the female sexual partners. Caucasian women have reported finding circumcised penises more sexually attractive, and at least some groups of African and Caucasian women have reported they would rather have sex with circumcised men. This is particularly true in relation to oral sex. However, results of the Australian study of sexual practice showed no significant differences in the proportions of circumcised and uncircumcised men who received fellatio or oral sex from their partners.
Limitations
There are a number of limitations of male circumcision, in relation to the health risks that the procedure brings about. While circumcision reduces the risk of some conditions of the genito-urinary system it does not eliminate the risk. Circumcised men who have unprotected sex are still at risk of contracting STIs, including HIV. Similarly circumcised boys may still experience urinary tract infections, however they are less likely to do so than uncircumcised boys.
Ethical considerations surrounding male circumcision

However to complicate matters, parents have internationally recognised rights, indeed obligations, to make medical decisions on behalf of their children. Parents equally have a responsibility to make decisions which are in the best interests of the child, but also have their own rights, for example to raise their child according to a set of religious beliefs. Weighing up the various social and biomedical factors which will affect the child, in order to determine what is in the child’s best interests, is therefore a complex process.
When the ethical issues are examined through a purely biomedical framework (i.e. considering health risk and benefit only and not social consequences), circumcision of infant and young males is generally considered unethical. Most of the health benefits of circumcision do not arise until adolescence or adulthood, when men and boys would be old enough to make their own informed decision about getting circumcised. On the contrary, some medical practitioners argue that there is mounting evidence of the health benefits of circumcision, and that when considered collectively, the benefits associated with circumcision outweigh the risk. Others argue that the risks of the surgical procedure are sufficiently low that parents should be able to decide whether or not to have their sons circumcised.
Other practitioners address the question from a broader framework and consider both the medical and non-medical benefits of the surgery. They highlight the need to recognise that individuals inherently believe in their own morals and that it is through their own moral framework that they make judgements about the value and harm in procedures such as circumcision. As every individual has a different set of moral beliefs, all individuals will come to different conclusions about what is good and bad. Given that there are numerous opinions about the relative harm and value of circumcision, the best interests of the child need to be established through the parents’ ethical framework and not that of the medical practitioners.
In Australia, the rights of parents are recognised, and while routine infant circumcision is opposed by professional bodies, their guidelines include provisions for circumcision under anaesthesia with parental consent.
More information
 |
For more information about circumcision, including the procedure and making the decision to circumcise, see Circumcision. |
References
- Marieb EN, Hoehn KN. Anatomy and Physiology (3rd edition). San Francisco: Pearson Benjamin Cummings; 2008. [Book]
- Holman JR, Stuessi KA. Adult circumcision. Am Fam Physician. 1999;59(6):1514-8. [Abstract | Full text]
- Policy statement on circumcision [online]. Sydney, NSW: Royal Australasian College of Physicians; 2004 [cited 16 June 2009]. Available from: URL link
- New data on male circumcision and HIV prevention: Policy and programme implications, Conclusions and recommendations [online]. Geneva: UNAIDS; 28 March 2007 [cited 15 April 2009]. Available from: URL link
- McDonald A (ed). HIV/AIDS, viral hepatitis and sexually transmissible infections in Australia: Annual Surveillance Report 2008 [online]. Sydney, NSW: University of New South Wales; 2008 [cited 15 April 2009]. Available from: URL link
- Rennie S, Muula AS, Westreich D. Male circumcision and HIV prevention: Ethical, medical and public health tradeoffs in low-income countries. J Med Ethics. 2007;33(6):357-61. [Abstract | Full text]
- Weiss HA, Thomas SL, Munabi SK, Hayes RJ. Male circumcision and risk of syphilis, chancroid, and genital herpes: A systematic review and meta-analysis. Sex Transm Infect. 2006;82(2):101-10. [Abstract | Full text]
- Moses S, Bailey RC, Ronald AR. Male circumcision: Assessment of health benefits and risks. Sex Transm Infect. 1998;74(5):368-73. [Abstract | Full text]
- Vincent L. ‘Boys will be boys’: Traditional Xhosa male circumcision, HIV and sexual socialisation in contemporary South Africa. Cult Health Sex. 2008;10(5):431-46. [Abstract]
- Szabo R, Short RV. How does male circumcision protect against HIV infection? BMJ. 2000;320(7249):1592-4. [Abstract | Full text]
- Belmaine SP. Circumcision. Med J Aust. 1971;1:1148. [Full text]
- Richters J, Smith AM, de Visser RO, et al. Circumcision in Australia: Prevalence and effects on sexual health. Int J STD AIDS. 2006;17(8):547-54. [Abstract]
- Cold CJ, Taylor JR. The prepuce. BJU Int. 1999;83(Suppl 1):34-44. [Abstract]
- Circumcision policy statement. American Academy of Pediatrics. Task Force on Circumcision. Pediatrics. 1999;103(3):686-93. [Abstract | Full text]
- Adami HO, Trichopoulos D. Cervical cancer and the elusive male factor. N Engl J Med. 2002;346(15):1160-1. [Abstract]
- Castellsagué X, Bosch FX, Muñoz N, et al. Male circumcision, penile human papillomavirus infection, and cervical cancer in female partners. N Engl J Med. 2002;346(15):1105-12. [Abstract | Full text]
- Singh-Grewal D, Macdessi J, Craig J. Circumcision for the prevention of urinary tract infection in boys: A systematic review of randomised trials and observational studies. Arch Dis Child. 2005;90(8):853-8. [Abstract | Full text]
- Position statement: Routine circumcision of normal male infants and boys [online]. Parkville, Victoria: Australian College of Paediatrics; 1996 [cited 25 July 2009]. Available from: URL link
- Auvert B, Taljaard D, Lagarde E, et al. Randomized, controlled intervention trial of male circumcision for reduction of HIV infection risk: The ANRS 1265 Trial. PLoS Med. 2005;2(11):e298. [Abstract | Full text]
- Bailey RC, Moses S, Parker CB, et al. Male circumcision for HIV prevention in young men in Kisumu, Kenya: A randomised controlled trial. Lancet. 2007;369(9562):643-56. [Abstract]
- Gray RH, Kigozi G, Serwadda D, et al. Male circumcision for HIV prevention in men in Rakai, Uganda: A randomised trial. Lancet. 2007;369(9562):657-66. [Abstract]
- Millett GA, Flores SA, Marks G, et al. Circumcision status and risk of HIV and sexually transmitted infections among men who have sex with men: A meta-analysis. JAMA. 2008;300(14):1674-84. [Abstract | Full text]
- Aitken S, Allen K, Berzins K, et al. National management guidelines for sexually transmissible infections [online]. Melbourne, VIC: Sexual Health Society of Victoria; 2008 [cited 25 July 2009]. Available from: URL link
- Berer M. Male circumcision for HIV prevention: Perspectives on gender and sexuality. Reprod Health Matters. 2007;15(29):45-8. [Abstract]
- Viens AM. Value judgment, harm and religious liberty. J Med Ethics. 2004;30(3):241-7. [Abstract | Full text]
- Schoen EJ. Ignoring evidence of circumcision benefits. Pediatrics. 2006;118(1):385-7. [Abstract | Full text]
- Leitch IOW. Circumcision: A continuing enigma. Aust Paediatr J. 1970;6(1):59-65. [Full text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







