- What is Chicken Pox (Varicella Zoster Virus)
- Statistics on Chicken Pox (Varicella Zoster Virus)
- Risk Factors for Chicken Pox (Varicella Zoster Virus)
- Progression of Chicken Pox (Varicella Zoster Virus)
- Symptoms of Chicken Pox (Varicella Zoster Virus)
- Clinical Examination of Chicken Pox (Varicella Zoster Virus)
- How is Chicken Pox (Varicella Zoster Virus) Diagnosed?
- Prognosis of Chicken Pox (Varicella Zoster Virus)
- How is Chicken Pox (Varicella Zoster Virus) Treated?
- Chicken Pox (Varicella Zoster Virus) References
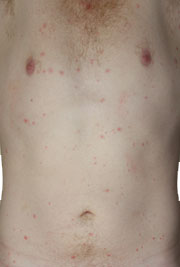
What is Chicken Pox (Varicella Zoster Virus)
| Chicken pox or varicella is an itchy, red, lumpy rash that is caused by the varicella virus. The Chicken pox virus is highly contagious for those who are not immune to it. You can only become immune to Chicken pox through already having the disease and developing antibodies to it or through vaccination, which has only been introduced in the last decade.Chicken pox is thought of as a common and fairly harmless childhood illness. The direct symptoms of chicken pox cause some discomfort without any complications. However, rarely the disease will predispose people to quite serious conditions that can occur at the disease onset or years later. Once a person has developed chicken pox the virus that causes the illness never goes away but lies dormant in the dorsal column of the spinal cord. If this virus is reactivated later in life (most commonly decades later) a condition called shingles or herpes zoster can occur. It is for these reasons that a vaccine for the disease is worthwhile, however whether the vaccine reduces the risk of shingles has not yet been established. |
Statistics on Chicken Pox (Varicella Zoster Virus)
In terms of overall population incidence there have been quite dramatic changes in the past decade due to the introduction of the varicella vaccine (chicken pox vaccine). Before the vaccine was introduced, 83% of all 10–14 year olds in Australia were estimated to have contracted chicken pox at some stage of their lives, further increasing to 95.5% of all 40 year olds. The highest incidence in Australia was in the 0–4 age bracket, with an annual rate of 78/100,000 for indigenous Australians and 43/100,000 for non-indigenous Australians. After this age the rate decreased dramatically. There were 4 deaths from varicella in Australia between 2003 and 2005. Recent data has shown there has been significant decreases in varicella-related hospitalisations since this time and this can be attributed to the vaccine. However, accurate incidence data in Australia is yet to be determined.
After the varicella vaccine was introduced in the US, chicken pox was estimated to be reduced by 84%. Furthermore, the incidence of varicella complications, including death, decreased by 66%.
Approximately 5 years after the introduction of the vaccine there was an increased number of breakthrough varicella cases. Breakthrough varicella is a chicken pox infection which occurs between 42 days to 5 years after vaccination to the disease. It is caused by the virus which was used in the vaccine. The symptoms associated with breakthrough varicella are less severe than the symptoms of cases which occur when the infection is transmitted from an infected person and breakthrough infections are far less contagious. However, 25% of vaccinated individuals will experience breakthrough varicella symptoms that are similar to chicken pox.
The increasing number of breakthrough varicella infections was taken by health authorities as an indication that the immunity provided by the vaccine was diminishing over time. In order to increase the immunity provided by chicken pox infection, doctors started giving all people aged >14 years two doses of the vaccine (spaced at least two months apart) instead of one.
Chicken pox in children
Chicken pox is very much viewed as a childhood disease, understandably so with 95% of varicella cases occurring in people under the age of 20. 75% of people contract chicken pox before 12 years of age.
Chicken pox in adults
Less than 5% of adults are at risk of contracting chicken pox. Of these, younger adults are the most susceptible.
Approximately 1 in 2,000 pregnant women contract chicken pox, a statistic that is not expected to fall until the last of the non-vaccinated generation surpass the childbearing age.
Risk Factors for Chicken Pox (Varicella Zoster Virus)
Not having been vaccinated against varicella is a predisposing factor for the disease. For those that are vaccinated there is a risk of developing a less severe outbreak of the disease which is termed breakthrough varicella. Breakthrough varicella is no longer a risk 5 years after vaccination.
Before the vaccination became available, up to 95.5% of the population were estimated to have contracted chickenpox at some stage of their lives. This suggests that the only predisposing factor to the disease is catching it from someone else that has it; this can either occur via airborne transmission or from direct contact with lesions.
Immunocompromised patients with underlying disease factors or those requiring immunosuppressive therapies are more likely to experience complications as a result of varicella. The virus is more likely to spread to the lungs, liver, kidneys, heart or brain in those that have T-cell defects.
Symptoms of Chicken Pox (Varicella Zoster Virus)
The first symptoms of chicken pox include:
- Headache;
- Fever;
- A general feeling of body discomfort and body aches;
- Fatigue; and
- Irritability.
After 48 hours the characteristic symptom of chicken pox will have developed which is the itchy, red and lumpy rash on the face, torso and limbs. As many as 250 – 500 chicken pox blisters can develop.
The chicken pox rash contains many lesions which develop at different stages. New fluid filled blisters develop for the first seven days of rash progression. After a week the blisters will begin to dry up. The whole process can last up to 20 days.
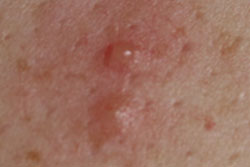
The lesions are small (less than 1 cm in diameter) and begin development as clear vesicles (fluid filled blisters) on an erythematous or “red” base. The vesicles then progress to pustules (pus filled blisters) and then crust over. The rash is highly contagious until all the lesions have crusted over.
The rash often spreads from a centre point and contains lesions at various stages of the rash progression.
How is Chicken Pox (Varicella Zoster Virus) Diagnosed?
Most chicken pox is very easy to diagnose. Doctors will enquire about exposure to the virus and the symptoms that were present before the onset of the rash, as many people will experience fever and a feeling of malaise before the visible onset of lesions. The rash is very itchy and the lesions are identifiable to a trained eye.
When a person presents with what appears to be chicken pox the doctor will need to establish a basic clinical history in order to determine whether the individual is at risk of further complications. The doctor will ask whether the infected individual is:
- Pregnant;
- Immunocompromised or has an underlying disease such as chronic cutaneous or pulmonary disorders that effect the immune system;
- Taking any type of immunosuppressive therapy; and
- Vaccinated against varicella – as this will determine whether the chickenpox is breakthrough disease.
For cases when the diagnosis is not clear, a sample of cerebrospinal fluid can be collected and subjected to tested using immunofluorescence or polymerase chain reaction (PCR). PCR can detect the varicella DNA while immunofluoresence detects the IgM antibody that is produced as a consequence of contracting the varicella virus, and hence both can provide confirmation that the individual is infected.
Prognosis of Chicken Pox (Varicella Zoster Virus)
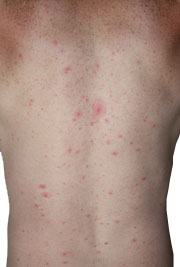
The most common complication for a vaccinated person is breakthrough disease. Breakthrough varicella occurred more commonly before the introduction of the second vaccine dose in 1995. However, it is still reported even in immunocompetent and highly vaccinated individuals.
Breakthrough varicella is defined as onset of chicken pox between 42 days to 5 years after vaccination to the disease. The symptoms associated with breakthrough varicella are less severe; with little or no fever and only around 50 skin lesions. The lesions that are present are usually maculopapular in nature, that is, a rash comprised of small red bumps instead of pustules and lesions. That said, 25% of individuals will experience breakthrough varicella symptoms that are similar to chicken pox. Breakthrough varicella is around 50% less contagious than chicken pox.
Before the chicken pox vaccine became available, the complications associated with chicken pox had greater prevalence, especially for immunocompromised individuals. This is not to say that immunocompetent individuals did not also carry the risk for the following:
- Otitis media;
- Subclinical hepatitis;
- Cerebellar ataxia; (inability to coordinate voluntary movements) and
- Bacterial superinfection of the rash.
Rare complications of varicella include:
- Encephalitis;
- Pancreatitis;
- Orchitis;
- Bleeding diathesis;
- Nephritis;
- Myocarditis;
- Pericarditis; and
- Cranial nerve palsies.
The risk of complications associated with chicken pox increases with increasing age of contracting the disease. If a woman contracts the disease when pregnant her child will have a 2% chance of developing congenital varicella syndrome which can have serious consequences for the developing baby including:
- Neurologic abnormalities such as brain atrophy or mental disability;
- Visual defects;
- Increased risk of developing shingles during infancy or childhood;
- Hypoplastic limbs; and
- Skin scarring.
How is Chicken Pox (Varicella Zoster Virus) Treated?
Chicken pox vaccine
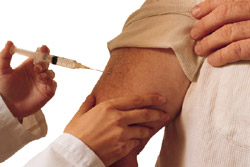
The major adverse events associated with the vaccine are rash, fever and injection-site reactions, all relatively minor and treatable.
At-home care
Once the varicella virus has been contracted treatment involves controlling the itch and keeping hydrated. It is important to remember to monitor children to make sure they avoid scratching the rash as much as possible. Basic, non-prescription non-allergenic creams, lotions and medications can be useful in calming the itch.
Both children and adults should stay at home once the rash has begun until all the blisters have dried up to avoid spreading the virus.
Special considerations
For those who have had significant exposure to the disease, are not immunised and are assessed to carry a high risk of developing severe varicella, an intramuscular varicella-zoster immune globulin (VZIG) can be administered within 96 hours in order to prevent chicken pox developing. VZIG is a preparation containing antibodies to the varicella virus.
Pregnancy

If chicken pox is contracted during pregnancy a dose of VZIG can reduce the severity and duration of symptoms if administered immediately (ideally within 72 hours) after the woman is exposed. If it is not possible to have the immunoglobulin injected within 72 hours, it may still provide some benefit if injected within 96 hours of chicken pox exposure. After the initial exposure VZIG will not be effective and will not be administered. Administering immunoglobulin to prevent chicken pox in pregnant women is very important because the medicines used to treat chicken pox, which come from a class of medicines known as antiretroviral agents, are not approved for use in pregnancy.
Newborns can also be treated prophylactically with VZIG if their mother contracted the infection at late stages of the pregnancy. These infants should be separated from other pregnant women and kept very well hydrated. If chicken pox does develop, antiviral agents such as oral acyclovir can be helpful to reduce the severity of the rash.
Skin conditions
Pre-existing skin conditions, such as eczema, may be further aggravated with some creams and lotions used to calm chicken pox. Make sure a doctor assesses the topical treatment prior to use to ensure they are appropriate and will not cause further irritation. The use of aspirin during chicken pox must be avoided as it has been associated with higher incidence of skin and soft tissue complications.
The use of nonsteroidal anti-inflammatory drugs should also be avoided as they have been associated with higher incidence of skin and soft tissue complications.
When to see a doctor
If you suspect that you or your child has been exposed to chicken pox or that the rash has begun to form see your doctor immediately. This is especially important for people with special considerations mentioned above.
More information
 |
For more information on chicken pox and related conditions, as well as some useful videos, see Chicken Pox, Shingles and Postherpetic Neuralgia. |
Chicken Pox (Varicella Zoster Virus) References
-
Masood SA, Kiel E, Akingbola O, et al. Cardiac tamponade and pleural effusion complicating varicella: A case report. Pediatr Emerg Care. 2008;24(11):777-81. Abstract
- Menzies R, Turnour C, Chiu C, McIntyre P. Vaccine preventable diseases and vaccination coverage in Aboriginal and Torres Strait Islander people, Australia 2003 to 2006. Commun Dis Intell. 2008;32(Suppl):S2-67. Abstract | Full text
- Macartney KK, Burgess MA. Varicella vaccination in Australia and New Zealand. J Infect Dis. 2008;197(Suppl 2):S191-5. Abstract | Full text
- Lee LE, Ho H, Lorber E, et al. Vaccine-era varicella epidemiology and vaccine effectiveness in a public elementary school population, 2002-2007. Pediatrics. 2008;121(6):e1548-54. Abstract | Full text
- Macartney KK, Beutels P, McIntyre P, Burgess MA. Varicella vaccination in Australia. J Paediatr Child Health. 2005;41(11):544-52. Abstract
- Karel DJ. Pruritic rash in pregnancy. Varicella virus. Am Fam Physician. 2009;79(5):405-6. Full text
- Adler AL, Casper C, Boeckh M, et al. An outbreak of varicella with likely breakthrough disease in a population of pediatric cancer patients. Infect Control Hosp Epidemiol. 2008;29(9):866-70. Abstract | Full text
- Farooqui AA, Tahir M, Jaiswal A, et al. Oculomotor palsy following varicella in an immunocompetent adult. South Med J. 2009;102(4):445. Full text
- Chickenpox (varicella) immunisation information [online]. Melbourne, VIC: Victorian Government Health Information; 28 August 2009 [cited 15 November 2009]. Available from: URL link
- Chickenpox – varicella [online]. Melbourne, VIC: Royal Children’s Hospital Melbourne; 2008 [cited 15 November 2009]. Available from: URL link
- Warshawsky B, Tan B, Deeks S. Advisory Committee Statement: VarizigTM as the varicella zoster immune globulin for the prevention of varicella in at-risk patients [online]. Ottawa, ON: Public Health Agency of Canada; 15 October 2006 [cited 30 October 2009]. Available from: URL link
- Heuchan AM, Isaacs D. The management of varicella-zoster virus exposure and infection in pregnancy and the newborn period. Med J Aust. 2001;174(6):288-92. Abstract | Full text
- Mikaeloff Y, Kezouh A, Suissa S. Nonsteroidal anti-inflammatory drug use and the risk of severe skin and soft tissue complications in patients with varicella or zoster disease. Br J Clin Pharmacol. 2008;65(2):203-9. Abstract | Full text
- National Foundation for Infectious Diseases: Facts About Chickenpox and Shingles for Adults [online]. NFID, 2009 [cited 24 Dec 2010]. Avaialble from: URL link
- Royal Australian and New Zealand College of Obstetricians and Gynaecologists. Antenatal screening tests. 2008. [cited 2010, Dec 28], Available from: URL link
- Australian Government Department of Health and Ageing and National Health and Medical Research Council. The Australian Immunisation Handbook. 9th ed. Updated July 2009. [cited 2010, Dec 28]. Available from: URL link
Drugs/Products Used in the Treatment of Chicken Pox:
- Aciclovir (Aciclovir)
- Varilrix Powder for Injection ( Varicella zoster vaccine, live attenuated )
- Varivax Refrigerated (Varicella zoster vaccine, live)
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.