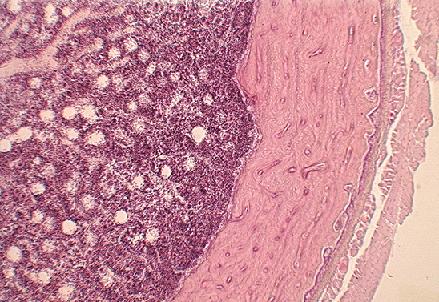
Bone marrow, a semi-liquid tissue found in the bone, is essential in the production of red blood cells, most white blood cells and platelets. A Bone marrow transplant is important in the treatment of blood disorders, such as acute leukaemias and other malignant disorders of the bone marrow. The patient’s (recipient’s) blood and defence systems are destroyed through chemotherapy and/or total body irradiation, and are then replaced by healthy bone marrow from an identical twin (syngeneic), a non-identical donor (allogeneic) or from the patient’s own bone marrow (autologous). This donor bone marrow is able to attach to the patient’s bone marrow, and can produce all the blood cells needed to replace the damaged patient’s cells. A Bone marrow transplant can have complications such as graft-versus-host disease, opportunistic infections, graft failure and relapse, and the procedure and follow-up requires specialised supervision by trained staff in fully equipped facilities. The histological image above is that of bone marrow with its constituent developing blood cells encased within compact bone.
Bone marrow, a semi-liquid tissue found in the bone, is essential in the production of red blood cells, most white blood cells and platelets. A Bone marrow transplant involves the destruction of the recipient’s own blood and immune defence systems by chemotherapy and/or total body irradiation followed by replacement with healthy bone marrow, either from either an identical twin (syngeneic), a non-identical donor (allogeneic) or from the patient’s own bone marrow (autologous). Its role in the management of various diseases depends on how severe the disease is, the type of disease, whether the cancer patient has improved (remission), the age of the cancer patient and the availability of appropriate bone marrow donors.
Type of bone marrow transplant
There are three categories of bone marrow transplant:
- Autologous: individual donates to themself.
- Syngeneic: transplant taken from identical twin.
- Allogeneic: transplant from an HLA-matched sibling or an unrelated HLA-matching donor (HLA = Human Leucocyte Antigen).
Allogenic transplantation uses cells taken from another person to reconstitute replace the blood and immune defence systems of the recipient. It has many complications, including further illness and even death. Autologous transplantation is useful when a cancer patient receives high dose chemotherapy/radiotherapy and needs replacement of their cells. It has fewer complications than allogenic transplants. However it can reintroduce malignant cells and the disease is more likely to come back with this bone marrow treatment. Autologous transplantation is also useful if the disorder does not initially affect the blood.
Indications
Allogenic bone marrow transplantation is indicated in disorders that affect the production of adequate and functional blood products. These disorders range from cancers that affect cells in bone marrow that are able to produce into all types of blood cells during cell development, such as acute leukaemias, to major inherited defects in blood cell production, such as thalassemia major.
Neoplastic disorders: Leukaemias:
- Acute lymphoblastic or myeloid leukaemia in first remission.
- Chronic myeloid leukaemia in chronic phase.
- Chronic lymphocytic leukaemia.
Other malignant disorders of bone marrow:
- Multiple myeloma, lymphoma, myelodysplasia.
Failure of haematopoiesis:
- Severe aplastic anaemia.
Major inherited disorders in blood cell production:
- Thalassaemia major.
- Sickle-cell anaemia.
Inborn errors of metabolism in haemopoietic and mesenchymal systems:
Autologous bone marrow transplant is indicated in acute and chronic leukaemias, multiple myeloma, severe autoimmune disease, amyloidosis and Hodgkin’s disease and non-Hodgkin’s lymphoma.
Stages of Bone Marrow Transplant
Conditioning: The conditioning stage involves the pre-treatment of the bone marrow transplant recipient with high doses of chemotherapy +/- total body irradiation to destroy the malignancy. This also damaged the recipient’s blood and immune defence system. Cyclophosphamide is the main bone marrow treatment used. Cyclophosphamide has complications, such as nausea, bleeding into the bladder (haemorrhagic cystitis), inflammation of mucosal surfaces and predisposition to infection. It may therefore be administered with antiemetics, mesna (to decrease the risk of haemorrhagic cystitis from the renal excretion of metabolites), parenteral nutrition and prophylactic oral antibiotics, antifungals and antivirals.
Bone marrow harvesting: Bone marrow is collected from the donor under general anaesthetic. 500 to 1200mL of marrow is harvested from the pelvis.
Processing: The bone marrow is then processed to remove red cells and to concentrate the mononuclear cells. Autologous transplants may be treated by chemotherapy or monoclonal antibodies to remove any cancer cells. Allogenic transplants may be treated with antibodies to remove T cells, to decrease the risk of graft-versus-host disease (GVHD).
Transplantation: Processed donor cells are injected into the recipient, where they find their way to the bone marrow and attach. There is a severe lack of bone marrow cells during this phase, lasting 1 to 3 weeks. During this period, the recipient requires intensive support therapy, including red blood cells and platelets and antibiotics. Those receiving allogenic transplants require prophylaxis against GVHD, such as cyclosporine +/- methotrexate. The bone marrow cells then begin to produce granulocytes, followed by an increase in red blood cell, platelet and white blood cell numbers. Sufficient numbers of these cells should be present after 3 to 4 weeks post-transplantation. Bone marrow reserve remains impaired for 1 to 2 years after the bone marrow transplant.
Complications
Complications with bone marrow cancer can be divided into early (<100 days post-transplantation) and late (>100 days), although many can develop during both stages.
Early complications with bone marrow cancer:
- Opportunistic infections – Especially bacterial, fungal, herpes simplex virus and cytomegalovirus.
- Acute graft-versus-host disease.
- Graft failure – Especially in aplastic anaemia.
- Haemorrhagic cystitis.
- Interstitial pneumonitis.
Late complications with bone marrow transplant:
Opportunistic infections – Especially varicella zoster virus and encapsulated bacteria.
- Chronic graft-versus-host disease.
- Chronic pulmonary disease.
- Autoimmune disorders.
- Cataracts.
- Infertility.
- Relapse of disease.
Opportunistic infections: During the initial post-transplant phase, recipients are more likely to get infections because of the damaged immune system. Cancer patients are especially predisposed to bacterial (Gram positive and Gram negative organisms), fungal (Candida and Aspergillus) and viral (herpes simplex virus) infections. This predisposition continues in GVHD or graft failure occurs.
Graft-versus-host disease: GVHD is due to the cell damaging activity of donor-derived immune cells, especially T-lymphocytes, which become sensitised to their new host and damage recipient tissues. This can vary from mild to lethal, and can cause serious morbidity or mortality. There is an increased incidence of GVHD with increased age of donor and recipient, and if there is any degree of HLA mismatch between them. Early GVHD affects the skin, liver and gastro-intestinal tract. A rash occurs, especially on the face, palms, soles and ears. Chronic GVHD involves not only the skin, liver and gastro-intestinal tract, but also the joints and other serosal surfaces, oral mucosa and lacrimal glands. This can lead to arthritis, malabsorption, hepatitis, scleroderma, sicca syndrome, lichen planus, pulmonary disease and serous effusions. Cancer Patients receiving allogenic transplants require prophylactic treatment for GVHD. This is usually cyclosporine (IV or orally for 6-12 months) and methotrexate (3-4 injections). Other options include the removal of T-cells from the donor bone marrow before infusion, or to give an anti-T cell antibody to the recipient. Early GVHD can usually be effectively treated with high dose corticosteroids. Chronic GVHD is more difficult to treat, and cyclosporine, azathioprine and corticosteroids are used, but responses are generally poor. The graft-versus-leukaemia effect is a paradoxical graft-versus-host effect where the donor immune system can help destroy the patient’s leukaemia by recognising the malignant cells and destroying them.
References
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







