- What is Atopic Keratoconjunctivitis (AKC)?
- Statistics
- Risk Factors
- Progression
- Symptoms
- Clinical Examination
- How is it Diagnosed
- Prognosis
- Treatment
- Atopic Keratoconjunctivitis (AKC) Prevention
- References
What is Atopic Keratoconjunctivitis (AKC)?
Conjunctivitis is a very common reason for experiencing an uncomfortable, red eye. There are a number of causes for conjunctivitis, including bacteria, viruses and, importantly, allergies. Allergic conjunctivitis affects the conjunctiva of the eye. The conjunctiva refers to the thin, translucent lining of the eyeball and the undersurface of the eyelids.
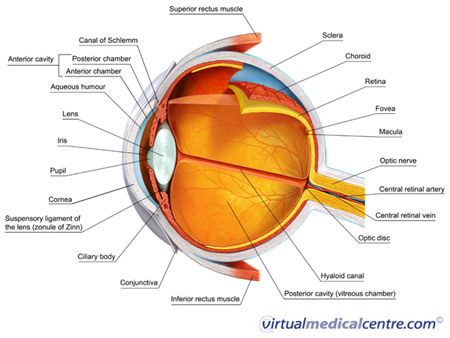
Atopic keratoconjunctivitis (AKC) refers to a particular type of allergic conjunctivitis. Commonly, both eyes are affected in AKC. It is strongly linked to atopic dermatitis (eczema).
Statistics
The majority of people who are affected by allergic conjunctivitis experience simple allergic conjunctivitis. The other forms of conjunctivitis such as AKC make up a small proportion of cases, estimated to be less than 1% of all eye allergies. AKC is rare, occurring in approximately 1 in 10,000 people.
The rate of AKC varies with the season and the country. For example, more people are affected in Italy, Japan and other warmer climates. It is also reported that AKC is more commonly experienced by males.
AKC is strongly associated with atopic dermatitis, which affects about 3% of the population. Of these people, it is estimated that 15–67% have some form of eye involvement, which is usually AKC.
Risk Factors

Family and personal history
A history of allergies is important, regardless of the type of allergic conjunctivitis. In particular, a history of atopic dermatitis and skin allergies in childhood is associated with the development of AKC in adulthood. About 95% of people with AKC report having had atopic dermatitis, while about 87% have experienced asthma earlier in life.
Age
Young adults are at the greatest risk of developing AKC. The condition occurs most frequently in people aged 20–50 years, and affects much fewer people past the age of 50.
Gender
The rate of AKC is higher in males than in females.
Symptoms
It is important that anyone with eye symptoms visits their doctor and provides a detailed clinical history. The doctor will rule out other types of conjunctivitis and more serious conditions that may cause uncomfortable red eyes.
The doctor will pay close attention to several aspects of your clinical history. In particular, they may ask:
- Have you had recent exposure to other people with conjunctivitis or an upper respiratory tract infection? This may suggest a viral cause of conjunctivitis.
- What are the details of your sexual history? In particular, have you had Chlamydia or Gonorrhoea? These can both cause conjunctivitis.
- Are you using any prescription or over-the-counter medications? Some medications can cause inflammation.
- Have you had any eye diseases before, used contact lenses, or had any other conditions that can be associated with eye conditions (e.g. rheumatoid arthritis)?
- Has anyone in your family had allergic conditions (e.g. hayfever, asthma or eczema)?
People affected by AKC will typically have itchy eyes, and often both eyes are affected. If itching is not present then allergic conjunctivitis is much less likely. Other eye symptoms such as blurred vision, burning, tearing and mucous discharge from the eyes may also be experienced.
If you have a red eye without itchiness, you may have a different eye condition. In this case, it is extremely important to seek medical advice from a doctor as soon as possible.
If you experience severe, continuous eye pain and reduced vision, promptly seek your doctor’s advice and you may need urgent referral to an ophthalmologist. These features are not typically present in allergic conjunctivitis and may point to a more serious eye condition.
Clinical Examination

The doctor may also use an ophthalmoscope to view the back of your eye, or a slit-lamp microscope to see the front structures of your eye. Both of these are painless, routine examinations.
How is it Diagnosed
Investigations are not usually required, as the diagnosis of AKC can be made on the basis of the clinical history and examination.
Prognosis
The prognosis and outcomes in AKC depend on whether the condition was treated and managed promptly or whether it progresses. If AKC is left untreated, it may result in ulcers and scars forming on the cornea, which may lead to vision loss in the most serious cases.
A small percentage of people (about 5%) with AKC develop a cataract due to the condition.
Treatment

Non-pharmacological therapy
Using a cool compress over the eyes and air-conditioning to cool the environment to an appropriate temperature may be helpful for AKC that is made worse by warmer environments.
Try to avoid rubbing or touching your eyes, as eye-rubbing may result in more inflammation.
Using eye lubricants and refrigerating eye drops may help soothe the eyes. Eye drops and lubricants dilute the factors that trigger allergic symptoms.
Pharmacological treatment
There are a number of different medications that can be used. The exact treatment plan will depend on how severe your symptoms are and what you may have already tried to treat your symptoms. In many cases, your immediate symptoms will be controlled with a short-term treatment program, followed by a longer-term maintenance plan. If you find your symptoms are not improving or are getting worse despite treatment, return to your doctor as soon as possible for a review.
Decongestants
The symptoms of allergic conjunctivitis arise because the chemicals released in response to the allergic trigger prompt a number of changes and inflammation. The small blood vessels in the eye enlarge, contributing to the redness, itchiness and discomfort experienced.
Decongestants are effective for several types of allergic conjunctivitis, including AKC, and are available in eye drop form. They keep the small blood vessels constricted, and in doing so, may provide some relief from allergic conjunctivitis. Side effects can occur if they are over-used or used for a long time, so they must be used following your doctor’s instructions.
Antihistamines

Short-term relief of the itching and redness can be provided by topical antihistamines and vasoconstricting eye drops.
Antihistamine agents attach to the same cells in your body as histamine, and in doing so prevent histamine from attaching to these cells. When there is a greater quantity of antihistamine, histamine is unable to bind to cells in the eye. As itching is only triggered when histamine binds to cells, antihistamines prevent or minimise the itchiness, redness and discomfort caused by histamine.
Mast cell stabilisers
Mast cell inhibiting medications stabilise cells in the eye known as mast cells, and in doing so prevent the release of histamine and other chemicals that cause the eyes to itch and swell. These medications are used to prevent allergic eye reactions. However, they do not provide immediate symptom relief.
Mast cell stabilisers are recommended for use year-round to control the symptoms of AKC. These medications are effective in most people and are generally safe but, like all medications, they should only be used according to your doctor’s advice.
NSAIDS
Topical NSAIDs may be considered in some cases of AKC, as they reduce itchiness and redness. NSAIDs do this by blocking enzymes involved in producing the chemicals that contribute to allergy and inflammation. Significant side effects can occur with NSAID use, so keep your doctor updated on how your treatment is progressing.
Corticosteroids
Corticosteroids are not recommended in all cases of allergic conjunctivitis, but are important in treating certain cases of AKC. They act by reducing inflammation, so they reduce the associated heat, swelling, pain and redness. They are usually applied to the surface of your eyelids, and as eye drops. Your doctor may suggest you start a course of steroids if you have tried other medications, but have not improved or your symptoms are worsening. It is important that steroids only be used for 1–2 weeks, under the supervision of an ophthalmologist and with regular review, due to the possible side effects including glaucoma, cataracts and corneal infections.
Steroids taken as a tablet may be necessary in severe cases of AKC, in which both eyes are involved or if your vision is affected. This may be an important method of treatment to prevent further complications and vision loss.
Cyclosporin
Cyclosporin binds to T-lymphocytes, preventing the production of chemicals involved in inflammation and thus reducing inflammatory and allergic symptoms. Cyclosporin may be useful in some cases of AKC that do not improve with other medications, such as mast-cell stabilisers and steroids.
These are powerful medications and should be used with caution and only following the instructions of your doctor due to potential side effects.
Antibiotics and antivirals
Treatment with medications that fight bacteria and viruses (antibiotics and antivirals) may be helpful because AKC is often accompanied by infections in the eyelid area. For example, infection of the eyelids is often caused by staphylococcus bacteria, so in these cases an appropriate antibiotics will be prescribed.
Surgery
Sometimes surgery may be necessary to treat AKC, for example to remove plaques that have formed on the cornea. However, this is not a common treatment strategy and would only be performed in certain cases after treatment with medications has been tried.
More information
 |
For more information about allergic conjunctivitis and its subtypes, see Allergic Conjunctivitis.
|
Atopic Keratoconjunctivitis (AKC) Prevention
The general principle for preventing all allergies is to avoid the triggers. Triggers for eye allergies can be avoided by:
- Using sunglasses to act as a barrier for airborne allergens;
- Using hypoallergenic bedding;
- Washing sheets in hot water; and
- Minimising animal exposure, if animals are believed to trigger allergic symptoms.
People who do not know what causes their allergic conjunctivitis may consider consulting an allergy specialist. The specialist may do allergy testing to find out what triggers the allergic symptoms.
References
- Khaw PT, Shah P, Elkington AR. ABC of Eyes (4th edition). London: BMJ Publishing Group; 2004. [Book]
- Leibowitz HM. The red eye. N Engl J Med. 2000;343(5):345-51. [Abstract]
- Bielory L, Friedlaender MH. Allergic conjunctivitis. Immunol Allergy Clin North Am. 2008;28(1):43-58. [Abstract]
- Khurana AK. Comprehensive Ophthalmology (4th edition). New Delhi: New Age International Publishers; 2007. [Book]
- Moloney G, McCluskey PJ. Classifying and managing allergic conjunctivitis. Medicine Today. 2007;8(11):16-21. [Full text]
- Schmid KL, Schmid LM. Ocular allergy: Causes and therapeutic options. Clin Exp Optom. 2000;83(5):257-70. [Abstract]
- Ono SJ, Abelson MB. Allergic conjunctivitis: Update on pathophysiology and prospects for future treatment. J Allergy Clin Immunol. 2005;115(1):118-22. [Abstract | Full text]
- Krachmer JH, Mannis MJ, Holland EJ. Cornea (2nd edition). China: Elsevier Mosby; 2005. [Book]
- Bonini S. Atopic keratoconjunctivitis. Allergy. 2004;59(Suppl 78):71-3. [Abstract]
- Bielory L, Mongia A. Current opinion of immunotherapy for ocular allergy. Curr Opin Allergy Clin Immunol. 2002;2(5):447-52. [Abstract]
- Bruce AS, Loughnan MS. Anterior Eye and Therapeutics A-Z. Philadelphia: Butterworth-Heinemann; 2003. [Book]
- Reinhard T, Larkin DFP. Cornea and External Eye Disease. New York: Springer Publishing; 2006. [Book]
- Smolin G, Foster CS, Azar DT, Dohlman CH. The Cornea: Scientific foundations and clinical practice. Philadelphia: Lippincott Williams and Wilkins; 2005. [Book]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







